Beukou Steve
Limbe, South-West Cameroon


Team HERO Cameroon organizing 2nd annual blood drive 2019 (Source: NGO HERO CAMEROON)

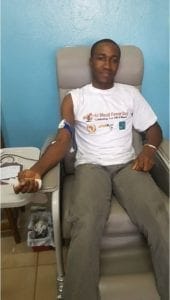
Team HERO Cameroon and voluntary blood donors during blood drive 2019 (Source: NGO HERO CAMEROON)
“Please I urgently need a donor who is blood group O rhesus negative for my sister to be operated. Please tell any of your friends.” These types of messages have become the newest type of notifications on our social media platforms in Cameroon. The notifications, while made up of different combinations of words, all convey the same message, which reflects the challenge of the lack of blood in our blood banks.
In 2019, the World Health Organization (WHO) reported 117.4 million blood donations, with more than half occurring in developed countries.1 That figure might seem huge, but when compared to the demand for blood, it looks insignificant. Mathematically, it is estimated that each country could individually meet its demand for blood, if 1% of the population donated to satisfy the needs.2 Paradoxically, with the thousands and millions of inhabitants in these countries, achieving just 2% of blood collection seems to be a fantasy for over 60% of countries worldwide.3
Similar to other global issues, the distribution of the demands and supply of blood is considerably asymmetric. The demand in developed nations is dominated by pathologies such as cancers, autoimmune diseases, and congenital anemia.3 Because of a pool of voluntary non-remunerated blood donors,4 patients suffering from these diseases are saved in emergencies or have a better quality of living. The other side of the mirror reflects an inversely proportional demand in developing countries from conditions such as post-partum hemorrhage, sickle cell anemia, motor-vehicle accidents, chronic kidney disease, and infectious disease.5 With the main pool of donors being family members, the reliability of a constant and regular supply of blood is very difficult as they constitute less than 50% of the donor pool.1 The direct consequence is an increase in the death toll with skyrocketing maternal mortality from post-partum hemorrhage and children unable to celebrate their fifth birthdays because of anemia from malnutrition and malaria among others. It is dumbfounding to realize that the same nations who require the most urgent action for blood donation, are also the least engaged in this life saving gesture.

It even more devastating to look at this complex and paradoxical concept under a magnifying lens. The irony of blood donation is that there are 32.6 blood donations per 1,000 people in high-income countries as compared with less than 5 blood donations per 1,000 people in low-income countries1 and extremes of 0.7 donations per 1,000 people in certain countries that are in dire need of blood.6 Even when the few altruistic and committed blood donors in developing regions answer the call of the blood bank, the high rate of blood-borne infections excludes the majority.7 Nevertheless, over the last two decades there has been a reduction in all infections except for Hepatitis B,8 owing to government-instituted public health interventions.
The wide disparity in the infrastructure, diagnostic techniques, and equipment used for blood donation further solidifies this paradox.9
Moreover, the burden of communicable and non-communicable diseases, poverty, cultural beliefs, ignorance, poor healthcare systems, and lack of universal health coverage in low-middle income countries (LMIC) and low-income countries (LIC) are additional challenges.10


Though a seemingly gloomy and hopeless situation, individuals, civil societies, and institutions have started advocating to address the need for blood. Globally there is a recognition of blood donors by the WHO each year on June 14th. Blood donation associations across the globe, international organizations like the Red Cross, and others respond to the need for blood. In the heart of Africa, a social enterprise called Blood Track and the non-profit NGO, Health Education and Research Organization (HERO) Cameroon are working toward a common goal, vision, and mission of improving the lives of both blood donors and recipients. Leveraging the recent developments in digital health technology, a sustained presence has been established online for advocacy on this issue. While HERO Cameroon focuses on organizing the blood donation campaigns, Blood Track follows-up with donors and focuses on community education to delete myths, misconceptions, and fictions surrounding blood donation. The work of these organizations over the last three years has resulted in more than 200 pints of whole blood collected from donors, over 5,000 people educated on the importance of blood donation, 600 familial blood donors converted to voluntary non-renumerated blood donors, and the provision of health insurance for donors who face health issues.
To better understand the perspective from the blood donors’ point of view, evidence-based research in the community is carried out to tailor community intervention. One such project has been the scientific work by HERO Cameroon titled “Knowledge, attitude and behaviour of blood donation among health science students in Cameroon” which is currently under scientific review.
Since the Second World War the availability of blood donors and blood donation has been capital in saving lives.11 Thus with measures such as community education, blood drives, and allocation of resources, the paradox of blood donation will eventually be rendered a historical memory.
Endnotes
- Blood safety and availability.World Health Organization,2019. Accessed January 13th, 2020. https://www.who.int/news-room/fact-sheets/detail/blood-safety-and-availability
- Blood safety and availability . Accessed May 12, 2019. Available from: https://www.who.int/news-room/fact-sheets/detail/blood-safety-and-availability
- Roberts Nicholas, Spencer James, Meghan Delaney. Global need and availability of blood products: a modelling study. The Lancet hematology,2019.
- Field SP, Allain J-P. Transfusion in sub-Saharan Africa: does a Western model fit? J Clin Pathol. 2007
- Dzik WS, Kyeyune D, Otekat G et al. Transfusion medicine in Sub-Saharan African:Conference summary. NCBI,2015.
- Andre L. Current Status on Blood safety and Availability in the WHO African Region-Report of the 2013 survey. Geneva: World Health Organization Regional Office for Africa. 2017
- Tagny CT, Mbanya D, Tapko J-B, Lefrère J-J. Blood safety in Sub-Saharan Africa: a multi-factorial problem. Transfusion (Paris). 2008
- Rerambiah Kouegnigan , Biyoghe AS, Bengone C, Djoba Siawaya JF. Evaluation of blood donors questionnaire in a developing country: The case of Gabon. Transfus Clin Biol. 2014
- Abu Noryati, Rama Bhatin, Kamul Bruket et al. Manual on management, maintenance and use of blood cold chain equipment . Pgs 15-44, 2005
- Claude Tagny, Laperche S, Murphy EL, Francophone Africa Network for Transfusion Medicine Research. Updated characteristics of blood services, donors and blood products in 11 French-speaking African countries. Vox Sang. 2018
- Schneider WH. History of Blood Transfusion in Sub-Saharan Africa. Transfus Med Rev. 2013
BEUKOU FONKOU HYGIN STEVE, MD, is a physician with a special interest in blood donation and research. In addition to scientific publications he works with the NGO Health Education and Research Organization (HERO) Cameroon. As blood drive coordinator he has overseen the donation of 200 pints of blood to the blood banks of his community over three years. Through the organization Blood Track, which he founded, these donors are followed-up to ensure regular, prompt, and safe blood donation.
