Camille Kroll
Chicago, Illinois, United States
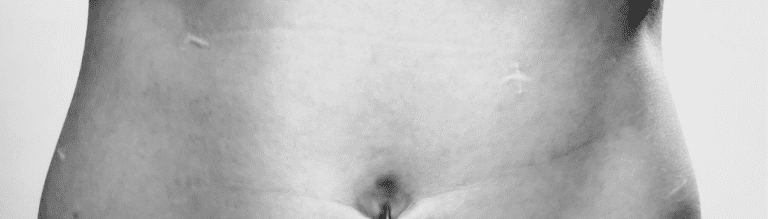
By Camille Kroll.
I was wheeled into the bright lights of the operating room with the symptom-based diagnoses of chronic pelvic pain and irritable bowel syndrome. When I groggily emerged several hours later, I had a new label: someone with a disease. Endometriosis is a notoriously tricky disease to diagnose because often only surgery can confirm its existence. It hides within the opaque body, requiring flesh to be sliced and peeled back to expose the spider’s web of adhesions pulling bowels and reproductive organs into a painful embrace. The gynecologist had felt an endometrioma during that fateful pelvic exam that rerouted my diagnostic trajectory.
I share my story not to malign the physicians who were unable to diagnose my disease. At a young age, I was told that as a woman, pain was inevitable. I normalized my pain within the frameworks I was given by my doctors, my family, other women, and the cultural forces that played such an important role in my meaning making. I was also told that my anxiety was not only worsening my symptoms, but also their nidus. The physicians too were working within biomedicine’s frameworks when they could find no obvious sign of disease.
I instead tell this story to show how my illness narrative was reimagined and I was given new freedom after being diagnosed with endometriosis, in part because of the relief and validation, both personal and social, that comes with a disease diagnosis. Looking at the glossy photos I received after surgery, I became a haruspex attempting to make sense of the bloody knotted organs before me. But instead of trying to tell the future, I retold the past as I amended my long-held illness narrative. I am reminded of psychiatrist and medical anthropologist Arthur Kleinman’s interview with a man suffering from chronic back pain: “[The surgeries] have created icons of his travail, scars that he can show people, that he can touch to assure himself that there is something ‘physically wrong.’”1
My illness narrative is intensely personal but also shaped and constrained by the cultural frameworks surrounding me. Culture affects how a person reacts to, experiences, and even narrates illness. Those who witness the ill individual’s suffering, including the person’s family, physicians, and the bureaucratic institutions that permit time off of work or disability benefits, collectively help to normalize certain expressions of illness, which then become the only acceptable expressions.2,3 Cultural masterplots, sometimes referred to as master narratives, frequently serve as frameworks for how people interpret their illnesses. Masterplots are deeply embedded within a culture and often reflect hegemonic values, such as the American success story that idealizes the hardworking, independent, and able-bodied individual.4,5 Contemporary Western medicine—and, specifically, biomedicine—helps to create these cultural narratives, while also being influenced by broader cultural forces, such as the neoliberal glorification of productivity and self-responsibility.6
A powerful narrative that biomedicine propagates is the elevation of disease over illness, which implicitly encourages questioning the suffering of individuals with chronic illness without diagnosed or diagnosable disease. Physicians value the concreteness of the physical lesion or quantifiable changes in biomarkers that disease represents. Illness, conversely, is experiential, and how symptoms become imbued with meaning is unique to patients and their social networks.7 Biomedicine sees all bodies as essentially the same, with aberrant physiological changes producing predictable effects. In this model, the subjective experience of illness can only be validated by the objective findings of disease. Thus, patients’ illnesses are often only legitimized if they can be mapped onto disease defined within the objective biomedical model.8
Chronic illnesses without diagnosed or diagnosable disease have many names: functional symptoms; somatization; somatoform; abnormal illness behavior; and medically unexplained symptoms, to name a few.9 Using psychiatric diagnoses to refer to persistent symptoms without an associated disease diagnosis highlights the limits of biomedicine’s epistemology when unable to explain a patient’s symptoms. These conditions do not neatly fit into the dualistic model of mind and body that biomedicine embraces. In fact, they might be considered “biomental” in that whether they are of the mind, body, or both often depends on whom you ask.10
Biomedicine’s privileging of illness associated with objective findings may seem natural because it has been normalized in Western culture.11 This seemingly normal elevation of disease over illness within the biomedical model has marginalized those with chronic illnesses without diagnosed or diagnosable diseases. Medical anthropologist Margaret Lock notes how the very peripheral status of a thing can empower it to question the norm: “Margins provide the Archimedian point . . . from where dominant ideologies—that which appears as normal and natural—can be scrutinized.”12
When confronted by chronic illness, individuals often experience what medical sociologist Arthur Frank has termed “narrative wreckage” as their life worlds and projected futures shift.13 In order to rebuild narrative coherence, they may turn to cultural masterplots, such as the powerful American narrative that one will be a responsible and productive patient by working toward recovery in order to again become a productive citizen.14,15,16 Biomedicine also perpetuates the narrative that disease is superior to illness and that—without a diagnosis of disease—one’s suffering may be questioned. These culturally-mediated understandings of what makes good patients, citizens, and—since being female significantly increases one’s likelihood of being diagnosed with a functional syndrome—women,17 shape these individuals’ illness experiences and the work they do to align their own stories with these narratives. Women suffering from chronic illnesses without diagnosed disease often perform extensive and tiring moral boundary work in order to prove to physicians that they belong to a “moral community” of deserving sufferers.18 Ideas of what being sick should look like pervade any medical encounter, but, for female patients, discourses of femininity, youth, and fertility also arise. Their suffering is often either minimized as an overreaction or normalized as the expected pain of being a woman.19,20,21,22,23
I can critique the culture of biomedicine while also recognizing that I ultimately benefited from the medicalization of my symptoms. In Western society, the need for a diagnosis of disease has strong cultural pull. Physicians have become powerful gatekeepers and agents of the state.24 The institutionalization of medicine has made diagnosis of disease the gate through which patients must pass for acceptance by their peers, as well as for access to medical care, coverage for that care, and application for state-sanctioned disability benefits.25
For a decade, I lived with the functional syndrome diagnoses of irritable bowel syndrome and chronic pelvic pain. Physicians attributed the former to my anxiety and the latter to normal variations in menstrual pain. When no disease was found, I turned to the cultural narratives that deemed my symptoms “normal” and “natural” products of my anxious constitution and female sex. I only began to question this tenuous narrative coherence when a pelvic exam revealed a small abnormal protrusion, leading to my disease diagnosis of endometriosis.
I was fortunate that the endometrioma betrayed the whole covert network otherwise I would never have been given a disease diagnosis; my chronic pelvic pain would have remained minimized as menstrual cramps fueled by an anxious disposition. The pain I had experienced for nearly a decade did not change the moment it received a new name, but its existence was validated. My narrative possibilities for giving meaning to that pain expanded once it was medicalized. The four thin scars now shine on my abdomen as a reminder of when the medical gaze fell on me and welcomed me into its biomedical narrative. My questionable illness was turned into culturally sanctioned disease and legitimized suffering. Medical management has even significantly improved my symptoms. Yet many will not be so lucky. The very existence of these suffering individuals exposes weaknesses in biomedicine’s epistemological framework and the cultural master narratives that we have normalized.
References
- Arthur Kleinman, The Illness Narratives: Suffering, Healing, and the Human Condition (Basic Books, 1988), 68.
- Kleinman.
- Charles E. Rosenberg, Our Present Complaint: American Medicine, Then and Now (Baltimore: Johns Hopkins University Press, 2009).
- H. Porter Abbott, The Cambridge Introduction to Narrative, 2nd ed. (Cambridge University Press, 2008).
- M. Cameron Hay, “Suffering in a Productive World: Chronic Illness, Visibility, and the Space Beyond Agency,” American Ethnologist 37, no. 2 (2010): 259-274, doi:10.1111/j.1548-1425.2010.01254.x.
- Hay.
- Kleinman.
- Michael Sharpe and Monica Greco, “Chronic Fatigue Syndrome and an Illness-Focused Approach to Care: Controversy, Morality and Paradox,” Medical Humanities 45, no. 2, (2019): 183-187, doi:10.1136/medhum-2018-011598.
- Richard Mayou and Andrew Farmer, “ABC of Psychological Medicine: Functional Somatic Symptoms and Syndromes,” Bmj 325, no. 7358, (March 2002): 265-268, doi:10.1136/bmj.325.7358.265.
- Joseph Dumit, “Illnesses You Have to Fight to Get: Facts as Forces in Uncertain, Emergent Illnesses,” Social Science & Medicine 62, no. 3 (2006): 578, doi:10.1016/j.socscimed.2005.06.018.
- Kleinman.
- Margaret Lock. “Contesting the Natural in Japan: Moral Dilemmas and Technologies of Dying,” Culture, Medicine and Psychiatry 19, no. 1 (1995): 1, doi:10.1007/bf01388247.
- Arthur W. Frank, The Wounded Storyteller: Body, Illness, and Ethics, 2nd ed. (Chicago: The University of Chicago Press, 2013), 53.
- Hay.
- Catherine Belling, A Condition of Doubt: the Meanings of Hypochondria, (Oxford University Press, 2012).
- Talcott Parsons, The Social System, (Glencoe: The Free Press, 1951; New Orleans: Quid Pro Books, 2012). Citations refer to the Quid Pro Books edition.
- Kirsti Malterud, “Symptoms as a Source of Medical Knowledge: Understanding Medically Unexplained Disorders in Women,” Family Medicine 32, no. 1 (2000): 603-611.
- Jane Pryma, “‘Even My Sister Says I’m Acting like a Crazy to Get a Check’: Race, Gender, and Moral Boundary-Work in Women’s Claims of Disabling Chronic Pain,” Social Science & Medicine 181 (2017): 66, doi:10.1016/j.socscimed.2017.03.048.
- Camille Kroll, “Questioning Biomedicine’s Privileging of Disease and Measurability,” AMA Journal of Ethics, 23, no. 7 (July 2021).
- Dumit.
- Olaug S. Lian and Catherine Robson, “‘It’s Incredible How Much I’ve Had to Fight.’ Negotiating Medical Uncertainty in Clinical Encounters,” International Journal of Qualitative Studies on Health and Well-Being, 12, no. 1 (2017), doi:10.1080/17482631.2017.1392219.
- Eva Lidén, Elisabeth Björk-Brämberg, and Staffan Svensson (MD), “The Meaning of Learning to Live with Medically Unexplained Symptoms as Narrated by Patients in Primary Care: A Phenomenological–Hermeneutic Study,” International Journal of Qualitative Studies on Health and Well-Being 10, no. 1 (2015), doi:10.3402/qhw.v10.27191.
- Pryma.
- Keith Wailoo, “Thinking Through the Pain,” Perspectives in Biology and Medicine 59, no. 2 (2016): 253-262, doi:10.1353/pbm.2017.0010.
- Rosenberg.
CAMILLE KROLL, MA, earned her master’s degree in medical humanities and bioethics from Northwestern University in Chicago, Illinois. She is currently pursuing her MPH at Washington University in St. Louis, Missouri. Her interests include the cultural study of biomedicine and biomedicine’s role in shaping Western master narratives about disease and illness.
