Alida Rol
Eugene, Oregon, United States
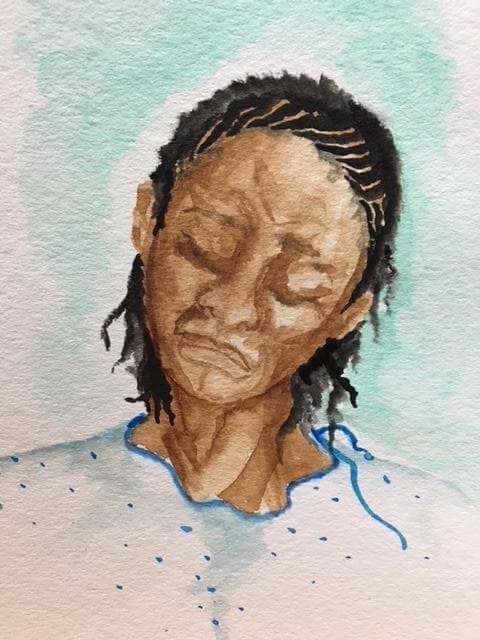 |
| Patient on the Table, 2017. Watercolor by Alida Rol, private collection. |
The world moves fast and it would rather pass u by than 2 stop and c what makes u cry.
– Tupac Shakur, “The Rose That Grew from Concrete”
She sits perched on the exam table in a too-large gown. We talk about a hysterectomy I have recommended, to remove the fibroid uterus that extends from its customary place in the pelvis to just beneath her ribs. She is in her late forties and has two grandchildren, yet she is tearful. This is not the first time we have met, nor is it the first time we have had this conversation. She is very polite when she tells me she just does not trust me. I am grateful for her honesty. And also hurt.
Two visits later and after a night of frightening pain, she consents to surgery—not as a woman offered relief but more like a suspect unjustly convicted. In the hospital she has no complications and never smiles. Unlike most patients, she never returns for a routine follow up visit after surgery.
Many years later, I think of her still. Though I sensed it from other women, she was the only one who said it aloud: “I just can’t trust you.” Because her distrust stays on my mind, I decide to write about it, imitating the vernacular she might have used. As the words hit the page, sincere and heartfelt, I pat myself on the back for my generous spirit. I have always treated everyone the same, I think. And then I read my piece in a writers’ group. We are all women. But for one writer who is Black, we are all White. The White women praise me one by one for capturing the patient so essentially, her words so realistically. The Black writer saves her critique for last, and with an exhausted voice tells me I have no right to put my White words in this Black woman’s mouth as though I understand who she is.
Tears prickle my eyes. My thin skin pales. The truth resonates in my gut.
Thus begins my education.
I do not have to look far or even look outside my own medical specialty. The “father of gynecology” is J. Marion Sims, whose statues and monuments dot Central Park and several southern states. Between 1845 and 1849 he experimented on young enslaved women in search of a cure for their fistulas, holes between the bladder and vagina, a complication of protracted childbirth. Fistulas left these women dripping urine, sometimes feces, the resulting odor intolerable, their skin raw. Sims operated on a young woman named Anarcha twenty-nine times before success with silver wire suture after the thirtieth attempt.1 This was before the days of widespread anesthetic use. One cannot speak of consent from the enslaved.
Over the last century and a half, physicians have continued to defend this slave owner’s “experiments” as appropriate for antebellum times. Some have insisted his means justify the ends, as the techniques Sims popularized continue to save women worldwide from an unbearable existence.2 Sims has been upheld in the profession as a physician to study and emulate. Charges of unethical practice have come primarily from non-medical quarters, especially historians and Civil Rights activists.3 But gynecology’s ignominious history does not begin or end with Sims, even if his practices set the tone. From the early 1900s until the 1970s, women were sterilized without their consent all over the country. These women were most often African American, Hispanic, Native American, cognitively impaired, or simply poor. They were told their tubes would be “tied,” implying an easy untying, or they were not told at all that a hysterectomy or tubal ligation had been performed. The secret procedure was so common, it was euphemistically referred to as a “Mississippi appendectomy.” Fannie Lou Hamer, a voters’ rights and Civil Rights icon, fell victim herself to such a hysterectomy at the hands of a White physician in 1961.
And then there was the much-vaunted scourge of “crack babies” who would, it was predicted in the 1980s and ‘90s, “overwhelm every social service delivery system” with their brain damage and antisocial behaviors. The crack epidemic was associated with Black communities, a view promoted by extensive and sensationalized media coverage.4 I remember a pregnant African-American patient who came to our maternity unit one night in 1992 with a blood pressure of 200/140. She was thirty-four weeks pregnant, a mother of two, and admitted to smoking crack cocaine. I was not surprised. We treated her and she made it uneventfully to term. Her case was flagged and her baby was placed in foster care. Not a month later, I admitted a White, well-spoken first-time mother at thirty-three weeks in preterm labor. The possibility of cocaine use never even crossed my mind until her urine drug screen, done by the nursing staff per protocol, came back positive. She took her baby home after its four-week stay in the neonatal intensive care unit.
Some pregnant women were actually criminally prosecuted, a manifestation of the “War on Drugs,” which led to the entirely disproportionate incarceration of African Americans. The crack-baby myth was later debunked with outcome data and less fanfare. Years later. Much less fanfare.5
Much has been written and said about race-based health disparities. A Black woman is more likely than a White woman to give birth prematurely, experience pregnancy complications, die as a result of childbirth, or lose her newborn. She finds herself more often pregnant unintentionally and may die sooner from cancer discovered at a later stage. Her life expectancy at birth is less than a White woman’s. We have grown numb to the bar graphs and statistics that favor White outcomes over Black ones. Yet when the Centers for Disease Control suggested a slight stagnation or dip in White life expectancy from 2015 numbers, concern and analysis saturated the airwaves and print pages.
Health disparities are frequently blamed on “lack of access to timely, appropriate, and high-quality medical care.”6 But what constitutes “appropriate” and “high-quality” and who decides that? If a patient looks at the entire medical system with suspicion, she may choose to delay accessing care even if (a big if) she has the means. Just this past summer, the National Institutes of Health partnered with a famous African-American church in Harlem to recruit participants for an ethnically inclusive health study.7 Black congregants were wary. They mentioned Tuskegee. Everyone remembers what happened in Tuskegee between 1932 and 1972. In a government study, Black men (and therefore their families) were left untreated for syphilis, unbeknownst to them and without their consent. The experiment did not end until it was exposed by the Associated Press.
Some congregants spoke of Henrietta Lacks whose cervical cancer cells were harvested without her knowledge or consent.8 To this day, letters from her name grace the human cell line most commonly used in human medical research. A forty-five-year-old graduate student, Hortensia Gooding, expressed this common sentiment: “There’s a lot of deep, deep-seated fear and concern that black lives don’t matter and that the medical community really will harm people of African descent on purpose—just for profit or just to help someone from another race.”9
How must it feel to be always wary, looking over one’s shoulder, at a time of medical need and vulnerability? Among possible remedies, an increased number of Black clinicians would seem logical and desirable. Yet this goal has for centuries been fraught with obstacles. In the days of slavery, midwives and healers from enslaved communities were disparaged and maligned. The enslaved were forbidden to read and write. After 1865, Blacks were prevented from attending “White” universities. Not so very long ago, in 1978, the Supreme Court of the United States ruled in favor of Allan Bakke, a White man who contested the affirmative action admissions policy of the University of California Medical School at Davis.10 While Black Americans make up 13.3% of the population, they have at most a 5.9% chance that their treating physician will be African American.11 What’s more, it now appears that a person’s perception of racial discrimination, alone, causes ill health.12
Belatedly, I must ask what I might have done to gain my patient’s trust all those years ago, the day she sat, head lowered, on the exam table. I might have listened, really listened, when she said she feared not being a woman anymore after a hysterectomy. I minimized her concern, dismissed it quickly, because I did not share her belief. Instead, I silenced her with a comment on her styled cornrows.
We will never know what Anarcha, Dr. Sims’ enslaved experimental subject, felt or thought. Before Sims sewed her up all those thirty times, Anarcha had been in labor for three days with her first child. Sims delivered her baby. He does not mention whether the baby lived or died, nor does he speculate whether his forceps delivery might have contributed to her fistulous injuries.13 Sims told his story, the preserved story, and mentioned Anarcha only when it suited his self-congratulatory purposes.
The few examples of systemic discrimination mentioned here barely scratch the surface of all those stories long untold. Acknowledging the sordid acts committed in the name of science and progress, and educating incoming students and practicing clinicians alike about this history, would go a long way towards increasing empathy and understanding in the workforce. Is it not incumbent upon the medical system to own up to its racist roots and denounce them—to broadcast the voices of the silenced? Silence is complicity. L-i-s-t-e-n is an anagram of s-i-l-e-n-t.
References
- Sims, J. Marion. The Story of My Life. New York: D. Appleton and Company, 1885. p. 227. p. 245.
- Wall, L L. “The Medical Ethics of Dr J Marion Sims: A Fresh Look at the Historical Record.” Journal of Medical Ethics 32.6 (2006): 346–350. PMC. Web. 20 Sept. 2017, and O’Leary, J. Patrick. “J. Marion Sims: A Defense of the Father of Gynecology.” Southern Medical Journal 97.5 (2004): 427-29.
- G. J. Barker-Benfield quoted in Kaiser, Irwin. American Journal of Obstetrics and Gynecology. 132:8. December 15, 1978. p.878-882; McGregor, Deborah K. From Midwives to Medicine: The Birth of American Gynecology. New Jersey: Rutgers University Press, 1998; Ojanuga, Durrenda. “The Medical Ethics of the ‘Father of Gynaecology’, Dr J Marion Sims.” Journal of Medical Ethics 19 (1993): 28-31.
- Okie, Susan. “The Epidemic That Wasn’t.” The New York Times 26 Jan. 2009. Health. nytimes.com. Web. 5 Oct. 2017.
- Frank DA, Augustyn M, Knight WG, Pell T, Zuckerman B. Growth, Development, and Behavior in Early Childhood Following Prenatal Cocaine Exposure: A Systematic Review. JAMA. 2001;285(12):1613–1625. doi:10.1001/jama.285.12.1613
- www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/cancer-facts-and-figures-for-african-americans/cancer-facts-and-figures-for-african-americans-2016-2018.pdf
- Stein, Rob. “Troubling History In Medical Research Still Fresh For African Americans.” All Things Considered. You, Me And Them: Experiencing Discrimination in America. NPR. 25 Oct. 2017. Radio. Transcript: www.npr.org/sections/health-shots/2017/10/25/556673640/scientists-work-to-overcome-legacy-of-tuskegee-study-henrietta-lacks
- Ibid.
- Ibid.
- Kendi, Ibram X. Stamped from the Beginning: The Definitive History of Racist Ideas in America. New York: Nation Books, 2016. pp. 425-428.
- aamcdiversityfactsandfigures.org/section-iv-additional-diversity-data/
- Lewis TT, Cogburn CD, Williams DR. Self-Reported Experiences of Discrimination and Health: Scientific Advances. Ongoing Controversies, and Emerging Issues. Annual Review of Clinical Psychology 2015 11:1, 407-440.
- Sims, J.M. p. 227.
ALIDA ROL, MD, MFA, practiced obstetrics and gynecology in Portland, Oregon, for nearly 25 years and retired to pursue her love of reading and writing. She obtained an MFA in creative writing and has had poems published in several journals. Her years in medicine continue to provide fodder for thought and creativity.
Highlighted in Frontispiece Volume 10, Issue 2 – Spring 2018
Winter 2018 | Sections | Doctors, Patients, & Diseases

Leave a Reply