Jayant Radhakrishnan
Chicago, Illinois, United States
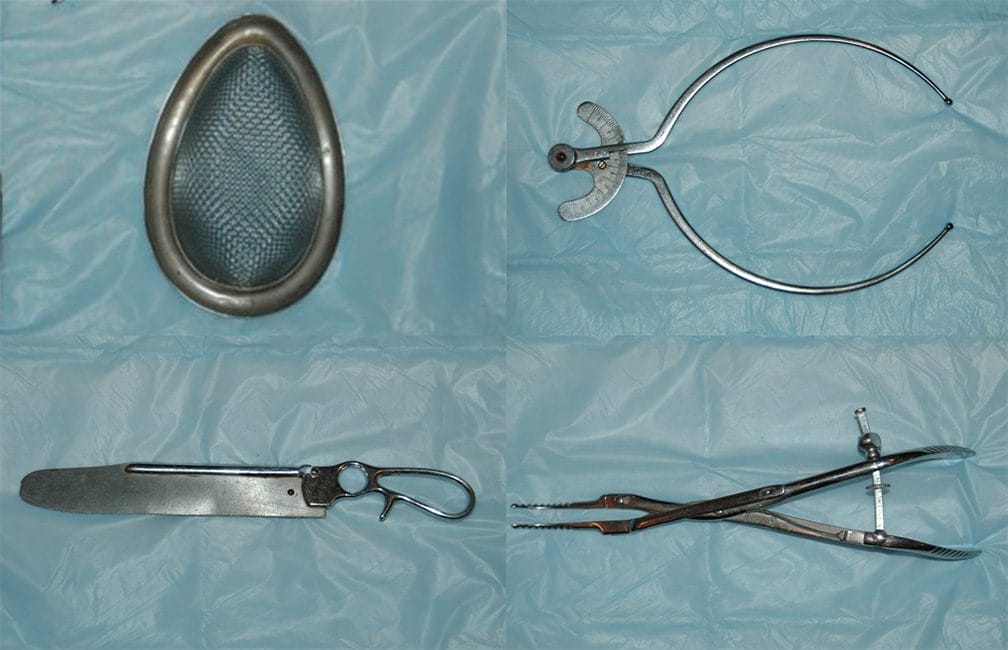
Photos by author.
Top left: Ether mask. After inducing anesthesia by spraying with ethyl chloride through the mask, ether was dripped through it to maintain anesthesia.
Bottom left: Bone saw.
Top right: External pelvimetry calipers. Dimensions of the false pelvis were measured. The pelvic inlet was calculated from that to determine if there was any cephalo-pelvic disproportion.
Bottom right: Cranial Trephine used following intrauterine fetal death to perforate the anterior fontanelle and evacuate brain matter. Collapsing the cranium permitted easier passage of the fetus through the birth canal.
Pain caused by surgical interventions is incorrectly considered an unimportant, self-limiting inconvenience. “Let them scream—it is a relief of nature,” said Benjamin Winslow Dudley, a professor of anatomy, surgery and medicine at Transylvania University, Lexington, Kentucky from 1817 to 1850. If Dudley’s unanesthetized patients squirmed during an operation, he would command, “Be still, Sir, or I’ll send your soul to Hell in half a second.”1
Dr. Dudley was a renowned surgeon and academician with a “quick and irascible” temper. In 1818, Dr. Daniel Drake questioned his autopsy techniques. Dudley was so insulted that he challenged Drake to a duel with pistols. Drake was against dueling to settle disagreements; therefore, his friend Dr. William H. Richardson took his place. The duelers positioned themselves at ten paces from each other on either side of the dividing line between two adjacent counties. Their positions in different jurisdictions made the duel legal. After they fired, Dudley was unharmed but Richardson sustained an exsanguinating groin wound. Richardson’s doctor could not control the bleeding so Dudley, with Richardson’s consent, sewed the bleeding artery and saved his opponent’s life. Supposedly, because of this duel, the American Medical Association was created to prevent doctor-upon-doctor murders.2
Because operations caused excruciating pain, surgeons disregarded precision, finesse, and safety in pursuit of speed. Robert Liston, the “fastest knife in the West End,” exemplified this approach. While preparing to operate, he would call out to observers, “Time me, gentlemen, time me!” If necessary, he held the bloody knife in his teeth to free both hands during the operation. He once amputated a leg in less than two and a half minutes, but he also removed his assistant’s finger and upon swinging the knife back, he cut a spectator’s coattails. The spectator promptly dropped dead from shock. The patient and the assistant both died of sepsis. Thus, Liston has the unique distinction of being the only surgeon with a 300% mortality from one operation. While amputating another man’s leg, Liston also excised his testicles.3
The Sumerians knew all about opium from about 3400 BC, but it only reached the Western world as a pain killer in the eighteenth century.4 In the United States, it was routinely used to control postoperative pain. It was not used during surgery for various reasons. Some thought it unethical to operate on unconscious individuals, while others believed that relieving pain delayed wound healing. Some religious writers opined that controlling pain violated God’s law.5 Dudley never explained his reasons for not treating pain.
Once the anesthetic value of ether and chloroform became apparent, surgeons used them but only for that segment of the population that they understood, could empathize with, and considered their equals. Racial prejudices and unfamiliarity with customs were major reasons for undertreatment of Native Americans and African Americans. They did not understand the Native American belief that withstanding physical pain led to resilience and not expressing distress was a sign of courage. Native Americans were even known to laugh when being tortured.6,7 African Americans were considered to be relatively insensitive to pain. Benjamin Moseley was possibly being laudatory when he wrote “…and what would have been the cause of insupportable pain to a white man, a Negro would almost disregard. I have amputated the legs of many Negroes, who have held the upper part of the limbs themselves.”8 Other studies claiming that African Americans did not feel pain and had thick skin were unquestionably meant to demean them and to claim superiority of the white race. Examples are the sadistic acts of violence that Thomas Hamilton committed on the slave Fed (who became John Brown upon escaping to England)9 and the preposterous theories of Samuel Cartwright regarding drapetomania (a disease that causes slaves to run away) and dysaesthesia aethiopica (partial insensibility of their skin).10 Surprisingly, these false perceptions still persist.11,12
The stellar reputation of J. Marion Sims, father of American gynecology, was ruined after recent reviews of his work deemed him a slave owner, a racist who experimented on slave women who were unable to consent to surgery, and a misogynist who operated on his patients repeatedly without anesthesia. Lastly, he turned them into drug addicts by using copious amounts of opioids postoperatively. While all the above are facts, there may be more benign explanations. He operated repeatedly because he was struggling with the extremely difficult problem of vesico-vaginal fistulae. He was the first person to cure these women. While slaves could not legally consent to surgery, he gave them detailed information about what to expect, and they cooperated in their own care. He once bought a slave because the owner would not give permission for her treatment. Opioids were routinely used for postoperative care at the time.13 He stated that he did not use anesthesia for operations on vesico-vaginal fistulae “because they are not painful enough to justify the trouble, and risk attending their administration.”14 He possibly made this ridiculous statement because ether and chloroform were not known early in his career. Therefore, he was unfamiliar and uncomfortable with their use when they were first introduced.
Surgeons quickly realized the benefits of not having a moving target during surgery and they progressively took to using anesthesia. However, some biases that persisted were “the meaning, rather than the fact of pain, was what mattered to the good life,” and regarding women in labor, that God inflicted pain during childbirth to “strengthen faith and to teach the mother the need for self-sacrifice for her children.”5
Charles Delucina Meigs (1792–1869), a leading American obstetrician of his time, was a staunch opponent of anesthesia during labor, in part because it impeded the progress of labor. He justified his stance by stating, “Few women lose their health or their lives in labor, and the dread of future sufferings is insufficient to prevent the increase of the family. As to the necessity of the Letheon practice [Morton’s name for his ether-based anesthetic product], the birth of the past myriads of the race shows that it is not necessary.”15 When the rich and famous, such as Queen Victoria, Mrs. Charles Dickens, and Mrs. Longfellow received anesthesia for childbirth, it became more acceptable but was administered based upon a “calculus” that determined “which patients were of the correct sensibility to need or benefit from the use of anesthesia.”5 By the late nineteenth century, general anesthesia was routinely used in surgery and even in labor—but not in neonates. They suffered for another 100 years.
Neonatal surgery became more commonplace after World War II, but anesthetic drugs and techniques effective and safe in adults turned out to be risky in neonates.16 Hence, the medical community disregarded centuries of observations that neonates felt pain. They chose to agree with Myrtle McGraw’s studies from 1941, which stated that babies did not require analgesia or anesthesia as their brains and nervous systems were undeveloped.17 Consequently, neonates undergoing surgery were intubated and given a muscle relaxant and oxygen. No anesthetic agent was administered. In the original Liverpool technique from which this method evolved, patients were anesthetized and muscle relaxants were not deemed necessary.18 This state of affairs persisted until 1987 when Kanwaljeet Anand in the UK demonstrated that pain caused marked physiologic changes during surgery.19 The Redbook, the Daily Mail (a British tabloid), and a member of Parliament pilloried him for demonstrating that neonates suffered during surgery. They neither understood his research nor that he was advocating for neonates to be anesthetized. The ensuing investigation by the UK General Medical Council not only exonerated him but went a step further and extolled the virtues of his work. Around that time, two mothers in the United States publicized their horror upon learning that their preterm babies had been operated upon without anesthesia.20 Studies have since established that while babies do not recall details later, the pain they were subjected to leaves a permanent mark on them, including both term and preterm babies.21,22 McGraw was grossly mistaken.
Close to the end of the twentieth century, the pendulum swung to the other extreme. In 1995, the president of the American Pain Society declared that pain was the fifth vital sign, even though it could not be verifiably measured.23 His statement, along with a letter from 1980 to the editor of the New England Journal of Medicine stating that short-term use of opiates in the hospital does not cause dependence,24 gave license to pharmaceutical manufacturers to push addictive drugs and for physicians to prescribe them liberally. Some physicians erroneously believed that the recommendations had a scientific basis. Others who worked for hospitals and medical conglomerates did so for self-preservation since pain control was now a metric in patient satisfaction surveys. Finally, for some, it was a financial windfall. The resultant excess of opioids prescribed for patients were sold on the streets and an epidemic of opioid dependence ensued. This morphed into a second wave consisting of heroin overdoses and then a third wave due to synthetic opioids such as fentanyl.
Postoperative opioids are still used in greater quantities in the US than abroad and American dosages are unrelated to the magnitude of the operation.25,26 Three recent studies tackling postoperative opioid use suggested that maximal immediate alleviation of acute pain resulted in minimal need for long-term pain control. One study demonstrated the value of an opioid-sparing postoperative pain management plan after minor surgical procedures.27 Another demonstrated that increased intraoperative use of fentanyl reduced the intensity of pain in the post-anesthesia care unit. In addition, “greater fentanyl administration was associated with decreased new chronic pain diagnoses at 3 months, decreased opioid prescriptions at 30, 90, and 180 days, and decreased new persistent opioid use, without significant increases in adverse effects.” On the other hand, hydromorphone had the opposite effect.28 The latest study employed rule-based guidelines for tailoring post-operative opioid prescriptions to in-hospital consumption.29
To date, management based on biases and ideologies has failed miserably; why not try science?
Bibliography
- Bullock WO. “Dr. Benjamin Winslow Dudley.” Annals of Medical History 7, no. 3 (1935): 201-213. Lexington Public Library. Accessed February 20, 2024.
- Hoover J. “The dueling doctors of Transylvania.” American Handgunner, 2022. https://americanhandgunner.com/discover/the-dueling-doctors-of-transylvania/. Accessed March 1, 2024.
- Gordon R. Great Medical Disasters. (Poughkeepsie: House of Stratus, 2001), 1-3.
- Encyclopedia Britannica. “Opium trade.” January 15, 2024, https://www.britannica.com/topic/opium-trade. Accessed March 20, 2024.
- Meldrum MC. “A capsule history of pain management.” JAMA 290, no. 18 (2003):2470-2475. doi: 10.1001/jama.290.18.2470.
- National Humanities Center Resource Toolbox. “European Americans and Native Americans View Each Other, 1700-1775.” https://nationalhumanitiescenter.org/pds/becomingamer/peoples/text3/indianscolonists.pdf. Accessed March 13, 2024.
- Sturycz C et al. “Qualitative Analysis of Pain Beliefs in Native Americans: Preliminary Findings.” The Journal of Pain 16, no. 4 (2015):S49.
- Moseley B. A treatise on tropical diseases; on military operations; and on the climate of the West Indies. (London: Strand, T. Caddel 2nd edition, 1789), 463-519. Digitized on the Internet Archive, 2014. https://archive.org/details/b21365234.
- Boney FN. “Doctor Thomas Hamilton: Two Views of a Gentleman of the Old South.” Phylon 28, no. 3 (3rd Qtr., 1967), 288-292. Published by: Clark Atlanta University. https://www.jstor.org/stable/273667
- Cartwright SA. “Report on the diseases and physical peculiarities of the Negro race.” New Orleans Medical and Surgical Journal 11 (1851):691-715. From DeBow’s review. Accessed March 14, 2024.
- Hoffman KM et al. “Racial Bias in Pain Assessment and Treatment Recommendations, and False Beliefs about Biological Differences between Blacks and Whites.” Proc Natl Acad Sci USA 113, no. 16 (2016):4296-4301. www.pnas.org/cgi/doi/10.1073/pnas.1516047113.
- Hoffman KM et al, “Supporting information,” in “Racial Bias,” 1-4. https://www.pnas.org/doi/10.1073/pnas.1516047113#supplementary-materials.
- Radhakrishnan J. “Presentism.” Hektoen International Physicians of Note Fall 2020. https://hekint.org/2020/12/30/presentism/
- Wall LL. “The medical ethics of Dr. J Marion Sims: A fresh look at the historical record.” J Med Ethics 32, no. 6 (2006):346-350. doi: 10.1136/jme.2005.012559.
- Meigs CD. Etherization in Obstetrics: The Science and the Art. (Philadelphia: Blanchard & Lea, 1856): 364-376. https://archive.org/details/obstartc00meig Accessed March 12, 2024.
- Rackow H et al. “Frequency of Cardiac Arrest Associated with Anesthesia in Infants and Children.” Pediatrics 28 (1961):697-704. PMID: 14489693.
- McGraw MB. (1943). In The Neuromuscular Maturation of the Human Infant. Ed. (New York: Hafner, 1963). Collection. Internet Archive.
- Rees GJ. “Anesthesia in the Newborn.” Brit Med J. 2 (Dec 23, 1950):1419-1422.
- Anand KJ et al. “Randomised Trial of Fentanyl Anesthesia in Preterm Babies Undergoing Surgery: Effects on the Stress Response.” Lancet 329, no. 8524 (1987):62-66. https://doi.org/10-1016/S0140-6736(87)91907-6.
- Anand KJS. “Discovering pain in newborn infants.” Anesthesiology 131, no. 2 (2019):392-395.
- Simons SHP et al. “Do We Still Hurt Newborn Babies? A Prospective Study of Procedural Pain and Analgesia in Neonates.” Arch Pediatr Adolesc Med. 157, no. 11 (2003):1058-1064. doi:10.1001/archpedi.157.11.1058.
- Selvanathan T et al. “Pain Exposure and Brain Connectivity in Preterm Infants.” JAMA Network Open 7, no. 3 (2024):e242551. doi:10.1001/jamanetworkopen.2024.2551.
- Campbell JN. “American Pain Society Presidential Address.” Pain Forum 5 (1996):85-88. doi:10.1016/S1082-3174(96)80076-6 Corpus ID: 72924729.
- Porter J, Jick H. “Letter to the Editor.” N Engl J Med. 302, no. 2 (1980):123. doi: 10.1056/nejm198001103020221.
- Lucas CE et al. “Kindness Kills: The Negative Impact of Pain as the Fifth Vital Sign.” J Am Coll Surg 205, no. 1 (2007):101-107. doi: 10.1016/j.jamcollsurg.2007.01.062.
- Brummett CM et al. “New Persistent Opioid Use after Minor and Major Surgical Procedures in US Adults.” JAMA Surg 152, no. 6 (2017):e170504. doi:10.1001/jamasurg.2017.0504.
- Hallway A et al. “Patient Satisfaction and Pain Control Using an Opioid-sparing Postoperative Pathway.” J Am Coll Surg 229 (2019):316-322. https://doi.org/10.1016/j.jamcollsurg.2019.04.020 ISSN 1072-7515/19.
- Santa Cruz Mercado LA et al. “Association of Intraoperative Opioid Administration with Postoperative Pain and Opioid Use.” JAMA Surg 158, no. 8 (2023):854-864. doi:10.1001/jamasurg.2023.2009.
- Beaulieu-Jones BR et al. “Postoperative Opioid Prescribing via Rule-based Guidelines Derived from In-hospital Consumption: An Assessment of Efficacy Based on Post-discharge Opioid Use.” J Amer Coll Surg (2024). Published ahead of print. March 25, 2024. doi: 10.1097/XCS.00000
JAYANT RADHAKRISHNAN, MBBS, MS (Surg), FACS, FAAP, completed a Pediatric Urology Fellowship at the Massachusetts General Hospital, Boston following a Surgery Residency and Fellowship in Pediatric Surgery at the Cook County Hospital. He returned to the County Hospital and worked as an attending pediatric surgeon and served as the Chief of Pediatric Urology. Later he worked at the University of Illinois, Chicago from where he retired as Professor of Surgery & Urology, and the Chief of Pediatric Surgery & Pediatric Urology. He has been an Emeritus Professor of Surgery and Urology at the University of Illinois since 2000.
