Jules Reich
Chicago, Illinois, United States
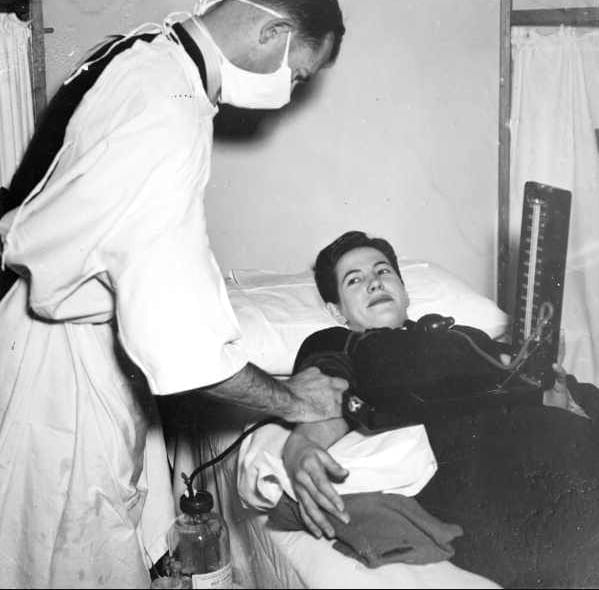
In 1937, the first U.S. blood bank opened in Chicago. It was originally called a Blood Preservation Laboratory, but its founder, Dr. Bernard Fantus, changed the name to blood bank. For someone who spent a large part of his exceptional career working on ways to make medicine taste better for children, this change made sense: it went down smoother. The term “bank” was not, initially, a metaphor.
In every sense, Fantus’s invention was a bank. It worked on the principle of separate, individual accounts with deposits and withdrawals. The blood bank functioned like a neighborhood bank. Healthy people were sent to participate in advance of need just as often as transfusion recipients were sent back to donate once they were healthy. It differed from a savings and loan institution only in that it was located in a hospital, and it held blood, not money.
Dr. Fantus encountered some difficulty in popularizing the bank, even within his profession. Doctors of the era were suspicious of his methods of preserving blood, and they were even suspicious of donors unrelated to recipients, whose motivations might be financial. Donors, on the other hand, underwent a painful process of opening a vein and risked infection. For patients who were generally healthy, and only feared needing a blood transfusion once in their lives, for some unforeseen major event, this worked well. They were able to supply the bank with blood when they were healthy, earning a credit, and know that if or when they ever needed it, they could withdraw from their account. People who withdrew from the bank to receive transfusions would be asked to make a donation in turn, either themselves when they became healthy, or by proxy through a friend or relative.
Into these dry facts, it is possible to read a variety of human stories. Having been denied a loan for a house or a small business, a resilient person could knock on a different door, wait for an upturn, move on to the next bank. A blood transfusion being withheld is a different matter entirely. For patients who routinely needed blood transfusion, for whom the painful process was needed to sustain life, the structure was burdensome. Rare was the hemophiliac with an endless list of healthy, local family and friends ready and willing to bleed. As time went on, and physicians began to take advantage of the ease of availability of the blood bank rather than the hassle and unreliability of donors, more and more blood bank donors were needed. Administrators had to rise to the challenge of encouraging hospitals to spend money on testing rather than just requesting Type O blood. They dealt with fears about transfusion between donors and recipients of different races, which at times were codified into law.
Without the strict accounting structure of the blood bank as originally conceived, some administrators were concerned that supplies would run out. They reasoned that people donated out of obligation, not out of altruism. Today, the vast majority of donated blood comes from donors who will never know or meet the recipients. Also, blood donation has become a simple, safe, and streamlined process, familiar to Americans through advertising and blood drives at their places of work and houses of worship. The “bank” in blood bank is now a reservoir, a collection and storage solution, rather than a means of accounting. Instead of discharging a debt, donors are seen as freely giving, connecting themselves to others without an expectation of what they will receive. Blood banking will likely continue to undergo changes and shifts for a long time to come.
JULES REICH is a writer interested in public health, medicine, and science. She is the host of the podcast It Turns Out. She lives in Chicago and graduated from Central European University in 2016.
Submitted for the 2019–2020 Blood Writing Contest
