Violet Kieu
Melbourne, Australia
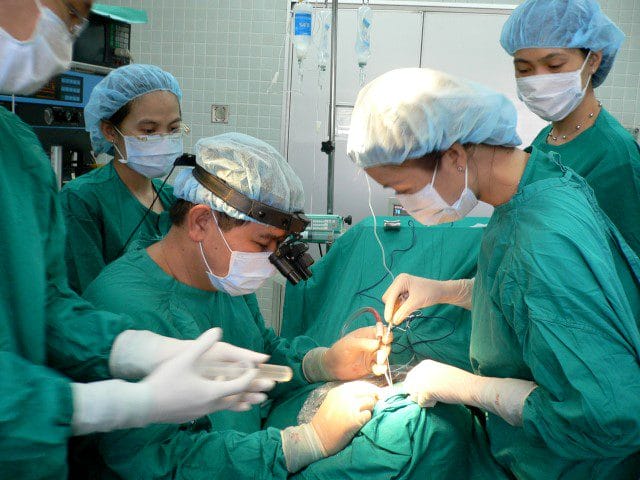
Photography by Violet Kieu
I was on a quest to become a surgeon.
Now I am simply on a quest to survive surgical training.
Getting into surgery was the easier part. Getting through, in comparison, is now the challenge. The very first year as a surgical registrar changed my life. It restructured my mental schema of self and reconfigured my definition of competence. I was broken down into component parts and rebuilt. I became more aware.
The stakes were high. Failure of the first part surgical exams meant dismissal from training. No arguments. Just anatomy, physiology, and pathology. If I passed, I promised myself freedom. This writing, then, is the anti-thesis of that time when surgery began to dominate my life.
I was rostered on for eight weeks of nights at a small peripheral hospital with a big catchment area. Needless to say, there were no silent nights. I was on call with a tough boss. One who took no nonsense and was ridiculously sensible.
‘As far as I’m concerned, breasts have only one purpose.’ I remember her saying. ‘To make milk.’
A remarkable lady of uncommon sense. These were her words, verbatim, from an impromptu tutorial on breast surgery. Obviously, I respected her. She taught me things. But what sort of teacher, and what sort of student, would we be on night duty?
The twilight drive to the hospital across town took a tedious hour to reach the residents’ quarters. The brick veneer room contained a bed, desk, chair, and lamp. All standard issue equipment. My companions of choice were single use packets of lube, disposable gloves, and a stethoscope. Some textbooks. Amongst the challenges one could expect to encounter were blood and shit and urine and coffee ground vomit and bile. For them, I wore the baby blue scrubs. I packed my pager, iPhone, and toothbrush.
All these objects were the symbols of a non-place.
I could have been in any hospital, anywhere. Who would have known the difference? The hospital, ubiquitous and purpose build, had an architectural philosophy of linear meaningfulness. A transitional, non-permanent space for treating patients.
This is not meant to be disrespectful. Rather, it acknowledges the challenge of turning the health system into a place of meaningful relationships, identity, and learning. To overcome the functional motif of hospital.
My identity was my job description, and it was new to me. Now I was the manager of abdominal pain in all its guts and glory.
Ring ring.
‘Are you the surg reg on call?’
‘Why, yes. Yes I am.’
The voice didn’t even ask for my name. I felt de-identified.
‘The ED consultant wants you down here. We have a rectal bleeder.’
‘Patient stable?’
‘Vitals normal.’
‘Hemoglobin?’
‘Bloods just sent.’
‘Sure. I’ll be down soon.’
I pushed aside my Last’s Anatomy and Ganong’s Physiology and entered the lonely corridor towards the Emergency Department.
‘Well, thank God you’re here,’ said the intern, as if we were in an episode of the eponymous comedy show. This was drama, I hoped not a tragedy, and perhaps the only comic relief was the impending conversation with my consultant. But first, I told the intern my name.
‘Hi, I’ve got a little old lady with PR bleeding.’
I saw the patient and called the surgeon.
‘Right. What does the rigid sig show?’
‘I haven’t done a rigid sigmoidoscopy.’
‘Why not?’
‘Because I’ve never done one before.’
Pause.
‘I can’t believe anyone can become a surgical registrar without being able to do a rigid sig,’ she said. ‘I’m coming in.’
As she hung up on me, I turned to the other mentor of my generation. Professor Google. How would you do a rigid sigmoidoscopy, sir? He boasted 66,000 answers within 0.19 seconds. But it was information without perspective, from the global stream of artificial intelligence. I YouTubed the procedure on my iPhone, bypassing hospital computer security that would not let me stream videos. Virtual reality and simulation training were all part of the new teaching armamentarium, but nothing could beat the real world experience of learning on the run.
I entered the cubicle, and consented the patient. The biggest risk, that of perforation. I showed her the plastic and steel instrument, as we waited for the boss to arrive.
‘I teach you because I care.’ The surgeon said. ‘So next time you can do it yourself.’
And with that wit, she instructed me to insert the instrument and look.
‘What do you see?,’ she asked.
‘It looks like hemorrhoids,’ I said.
‘What will you do?’
‘She’ll need an non-urgent colonoscopy.’
‘Good. You have to think like a surgeon.’
Teach a man to fish, a girl to operate, and you’ll have a fisherman and a competent registrar. A hungry man and a dangerous surgeon are best avoided. As a mentor she taught me how to learn by doing.
While I needed to study the texts to pass my exam, genuine teaching was happening now. In real life. See one, do one, teach one. But it was so much more than that. See many, do many, teach many. And reflect at each stage of the game. Experiential learning.
An age-old adage is that the ideal surgeon has the eyes of an eagle, heart of a lion and hands of a woman. They are sharp, determined, and skillful. But what does it mean to be a good surgeon in modern society? We have surgical competencies, a code of conduct, public opinion, the letter of the law. The aim now is to be a safe, independent practitioner. With emphasis on the individual’s desire to learn and ability to critique. To know our limits, make a decision, and call for help.
We also need to celebrate the small wins. Like our first rigid sigmoidoscopy.
As she left, I went back to my room and picked up a cold can of Coke from the vending machine. Splendid. Then the pager went off. Surgical registrar needed in Resus Bay 1.
Another little old lady. This time, a Jehovah’s Witness who was bleeding. My recently gained skills of rigid sigmoidoscopy were not so useful here. The haemorrhage was too much. What to do? Common sense and call for help. Anaesthetics, surgery, interventional radiology.
Think like a surgeon, she had said to me. This woman was dying. But it was not my knowledge I had to search, but my values. I was sad. She could not be resuscitated adequately; she was just bleeding too much. She would die.
You can operate until your arms drop off, but you need a reason why. First, do no harm. Do not do unnecessary procedures. You need to double check, triple check and cross check your decision making process. The choice not to operate weighs so heavily on the mind, when the outcome is the opposite of life.
Both patients and doctors need to know how to make the hard decisions, and live or die with the consequences. She passed away according to her beliefs, without heroics, but with dignity.
There are surgical success stories too. At another small hospital I met another boss. Same apprentice, different master. We learn how to become surgeons by thinking, through mentors, and not just by operating.
‘Hi, I’ve got a little old lady with massive PR bleeding.’
‘What does the CT show?’
‘No obvious bleeder.’
‘Well you know what you need to do.’
I did. Admit. Resuscitate. Transfuse.
He was a more laissez faire consultant and I added him to my mosaic of mentors. The hands-off approach gave me the chance to take responsibility and reassess. Things changed fast. The patient bled again. The CT angiogram was repeated and a bleeder was found. With flashing lights the patient was transferred to the interventional radiology suite.
She lived. I learned. I also passed my exams.
I studied my anatomy by night, so I could operate by day, to find meaningfulness in my work. I learnt that in all likelihood this craft is only going to get tougher, but, perhaps, so will I.
It’s a journey to find one’s own trajectory from novice to expert. The alchemy of attitude is required to turn any non-place into unique learning environment. The input of hours magicked into the output of patient care.
VIOLET KIEU is a writer and doctor from Melbourne, Australia. She has been published in Peril and Cha. Her writing has received a Boroondara Literary Award and has been shortlisted for the Marjorie Barnard Short Story Award from the Fellowship of Australian Writers. Violet is a trainee in obstetrics & gynecology with experience in pediatric & adult general surgery.
Highlighted in Frontispiece Volume 8, Issue 1 – Winter 2016
