Philip R. Liebson
Chicago, Illinois, United States
What constitutes a high-tech instrument? Obviously, in the field of medicine, one that has been developed to improve evaluation of a given condition and lead to a more specific diagnosis. In the early 19th century, there was little that could be considered high-tech in medicine in regard to instrumentation. The physician’s primary means of examining the chest were observation, palpation, and percussion. Actually, percussion of the chest was a novelty of the late 18th century, first developed by Leopold Auenbrugger, an Austrian physician; however, by the end of the century, it had fallen out of favor, except where it had been reintroduced by Nicolas Corvisart, Napoleon’s physician.
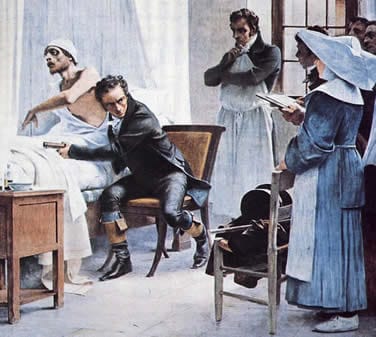
It would be expected that a willing student of Corvisart might make inroads into the examination of the chest, especially one who became fascinated with diseases of the chest after seeing his mother die of pulmonary tuberculosis at age six. Thus we introduce René Laënnec (1781-1826). Laënnec, like diagnosticians of the 19th century, was an astute observer. At the time, physicians “listened” to the chest by placing a handkerchief on the chest and then touching the ear to the handkerchief. Do not sneer at this method: as late as the 1920s and 1930s, one of the best cardiology diagnosticians, Lewis Atterbury Conner of Cornell Medical School, used this technique when he became so hard of hearing he could no longer use a stethoscope.
Laënnec, who had studied at the École de Medicin in Paris, had been taught the lost art of percussion by Corvisart. However, he found the use of auscultation with the aid of a handkerchief to be an awkward and frustrating experience, especially when examining obese women. Laënnec, being an observant fellow, noticed children playing with long hollow sticks and when the ear was placed at one end of the stick and a pin scratched at the other end the sound was amplified. Laënnec tried this by using rolled up paper, but also found this somewhat awkward. He was somewhat into carpentry and built a hollow wooden cylinder, 25 cm in length and 2.5 cm in diameter. Thus, a high-tech instrument was borne in the stethoscope. This he accomplished in 1816, while Napoleon, after a quick sojourn at Elba, was now permanently residing in St. Helena. Even though the word “revolution” was out of favor at that time, there is no other term that adequately conveys the import of this discovery; indeed, it had a longer-lasting impact than many of the ideas thought up by the men of the tumbrils several decades before.
Laënnec coined the term “stethoscope” from the Greek words for “chest” and “observer.” He also coined the term “mediate auscultation,” in that the instrument amplified sounds from the chest. His work included descriptions of auscultatory findings in various conditions previously difficult to discern, and introduced the terms such as râles, crepitance, egophony, and rhonchi. Initially, when evaluating heart sounds, he considered that S1 was produced by ventricular systole and S2 to atrial contraction rather than due to closing of the A-V valves and the valves to the great vessels, respectively. His landmark work, published in 1819, was entitled De l’Auscultation Médiate ou Traité du Diagnostic des Maladies des Poumons et du Coeur (On Mediate Auscultation or Treatise on the Diagnosis of the Diseases of the Lungs and Heart).
Let’s step back a minute. In order to fully appreciate Laënnec’s career, one must better understand the times in which he lived. While he was living with his famous uncle, Guillaume-François Laënnec, professor of medicine at the University of Nantes, the French Revolution began. This in no way affected René, who in his pre-teens at the time. He enrolled at the Collège d’Oratorie and studied liberal arts, including religion, political science (one might wonder how the ongoing revolution affected the teaching of this subject), grammar, geography, Latin, verse, and prose. Peaceful life or not, there was a guillotine in Nantes stationed in a square just outside his home, and he had seen several isolated heads produced by that new state-of-the-art procedure invented by Dr. Guillotine to bring death on rapidly in deference to the suffering of the victim. I suppose you could say that it was the precursor of the microtome.
Laënnec began the study of medicine at the age of 14 at his uncle’s hospital in Nantes when the revolution was at its height, and in 1799, along with Napoleon, entered Paris to formally study medicine under Corvisart. I leave it to the reader to decide which one of the two had the greater influence on the 21st century in regard to the individual patient.
His first published work in 1802 was a report of a case of mitral valve calcification with left ventricular dilatation evaluated at autopsy. Just after he received his doctorate, he lectured on tuberculosis. At the time, involvement of the lung was termed phthisis, and he became a savior of lisping physicians by indicating that it was pulmonary tubercu losis. Following this, he spent five years lecturing on pathologic anatomy and doing some private practice. He was also an editor of the Journal de Medicine from 1805 to 1808, between the ages of 24 and 27.
After 1819, when he had published his great work on auscultation, one would have thought that this would incite a revolution in the medical field in France. Wrong! Unfortunately, there was no Robespierre or Marat in medicine to foster his ideas and indifference was the attitude among his colleagues. However, the rest of Europe was enthusiastic, and physicians came from all over the continent to the Necker Hospital to see Laënnec demonstrate his new instrument. There is no information available on whether they received CME credits or had drug reps in the adjoining rooms. His book, of course, was a sellout outside of France. Finally, his French colleagues accepted his talents and he was made a professor of medicine at the Collège de France in 1822 at age 41 and a member of the Academy of Medicine. Several years later he was made a knight of the Legion of Honor. In 1826, still only 45 years of age, he developed a cold followed by a throat infection and chest pains. He asked his nephew to listen to his chest and describe what he heard. Laënnec interpreted the findings as cavitary tuberculosis. This caused his death. He died before Chopin developed full-fledged tuberculosis, but it would be interesting to surmise what Laënnec could have accomplished had he been the composer’s physician. At least we would have had significantly more knowledge of the extent of his condition.
In his will, Laënnec bequeathed to his nephew all his scientific papers and his stethoscope, which he indicated was “the best part of my legacy.” In 1867 money was raised in Europe for a monument to him at the Paris Exposition the following year. The modern binaural stethoscope was invented in the 1850s and the rest, as they say, is history. Now every practicing doctor, except psychiatrists, pathologists, and perhaps some dermatologists, carries around a stethoscope, and, despite the availability of echocardiography, chest radiography, CT scanning, and MRI, may occasionally use it. It is unlikely that any of them carry around Napoleon’s picture.
References
- Willius FA, Keys TE. Classics of Cardiology, Volume One. René Théophile Hyacinthe Laënnec pp. 323-382. Dover Publications, New York. 1941
- Roguin A. René Theophile Hyacinthe Laënnec (1781-1826): The man behind the stenoscope. Clinical Medicine and Research 2006;4:230-235.
- Fayssoil A. René Laennec (1781-1826) and the invention of the stethoscope. Am J Cardiol 2009; 743-744
- Scherer JR. Before cardiac MRI: René Laennec (1781-1826) and the invention of the stethoscope. Cardiology Journal 2007;14:518-519.
- Tan SY, Yeow ME. Medicine in Stamps René Laennec (1781-1826): Inventor of the stethoscope. Singapore Med J 2005;46: 106-107.
PHILIP R. LIEBSON, MD, graduated from Columbia University and the State University of New York Downstate Medical Center. He received his cardiology training at Bellevue Hospital, New York and the New York Hospital Cornell Medical Center, where he also served as faculty for several years. A professor of medicine and preventive medicine, he has been on the faculty of Rush Medical College and Rush University Medical Center since 1972 and holds the McMullan-Eybel Chair of Excellence in Clinical Cardiology.
Highlighted in Frontispiece Volume 5, Issue 2 – Spring 2013 and Volume 16, Issue 4 – Fall 2024
