John Graham-Pole
Antigonish, Nova Scotia, Canada
In this essay, I reflect on my journey as a pediatric oncologist—from a time when childhood cancer was nearly always fatal to the gradual emergence of cures. Drawing on personal experiences with patients and their families, I examine the medical milestones, ethical complexities, and emotional burdens that shaped my career and my conscience. I try to reckon with the cost of medical progress and the shadow that healing often casts.
The early years
The first evidence that children’s cancer could respond to chemotherapy came in 1947 at Boston Children’s Hospital when pediatric pathologist Sidney Farber achieved a short-term remission of a two-year-old’s acute leukemia with the antifolate drug aminopterin. But it would be many years before long-term remissions were possible, let alone cures. The first child I ever treated was in 1968 as a pediatric resident—an eight-year-old girl with widespread neuroblastoma. She had a complete response to our chemotherapy regimen, which lasted for eight months before she suffered a widespread recurrence.
During those early years, it was all too often my task to tell parents their child’s cancer had recurred—a horribly painful duty. We had learned to use the best therapy available at initial diagnosis, so secondary treatment was almost certain to fail and to cause worse side effects. But these second-line drugs were vitally important to our research, because many of them would become part of our frontline treatment. Informed consent is especially hard in this setting because of the complexity of our research and the family’s emotional distress. Detailed explanation of our experimental treatments could readily conflict with our focus on family-centered care.
Cures were still decades away. My first patient during fellowship was a thirteen-year-old with acute leukemia who had received three different treatment protocols, each one achieving shorter and shorter remissions. We learned a great deal from her responses—or lack of them—to our increasingly experimental therapies. But would it console her parents today to know that thousands of children have now achieved long-term remissions and even cures? It gives me little solace to know that almost all the children I treated during the first half of my career died of their cancer despite my treatment. It was only during the second half of my career that a fast-growing number were cured as a result of what we had learned from our earlier experiments.
Experiments and hope
Because children respond more completely than adults to chemotherapy and are far more resilient, our treatments grew more and more intensive. In 1976, I established Britain’s first unit dedicated to childhood cancer—and at once ran afoul of the head nurse. I introduced an intensive regimen for a child with acute myeloblastic leukemia—a highly aggressive cancer only recently starting to yield to chemotherapy. I still remember her horror at the treatment I proposed:
“You are giving these poor parents quite unjustified hope, Doctor. No one has ever been cured of this form of cancer. You are simply condemning this little girl to unwarranted suffering. I wish to register my strongest objection to your proposed treatment!”
I had learned to pay good attention to nurses. They do not develop our treatment protocols, but they have to implement them, and care for the patients when they inevitably develop severe side effects. But I had been hired to test these experimental treatments, so I pressed on in the face of this senior nurse’s strong objections. It was touch-and-go for many weeks until the little girl responded completely and never looked back. To me, the end justified the means, but it could certainly have gone the other way, and she might well have died a miserable death from the side effects of my treatment, as did so many of my patients.
Ted and the transplant era
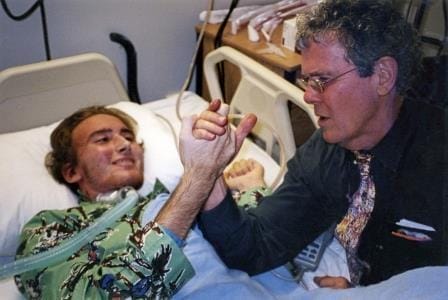
But what serendipity that I should have lived through this period when the success of chemotherapy for cancer emerged in full force. Because it was both the responsiveness of these young patients and their resilience to the horribly toxic drugs that finally led us to recognize that chemotherapy could cure cancer. In 1987, I was directing our bone marrow transplant center at the University of Florida when Ted Haines* came into my life. Thirty-eight years after I first met him, he turned up again to prompt me with old memories. Now approaching his fiftieth birthday, he emailed me with an update on his past four decades. He was blessed with that rarity of an identical sibling. Less than 30% of children have fully matched family members who can donate enough stem cells for a successful transplantation. Identical twins are a rarity—perhaps two percent of births, though such twinning has become more common with in vitro fertilization. It was Ted’s stroke of fortune that, when at the age of thirteen he developed B-cell leukemia, his brother was right there to become his bone marrow donor, because we believed that a stem cell transplant was the best treatment for his highly aggressive cancer.
Ted came through the transplant almost unscathed. I don’t remember those daily poker games he mentioned in his email, which he says I let him win, but I do know he would go on to become one of our early cures from bone marrow transplantation. Our treatment protocol of chemotherapy and total-body irradiation was the most intensive anyone could tolerate—and without an immediate infusion of stem cells Ted would never have recovered. He was cured of his cancer, and the price he paid—diabetes, thyroid, and neurological troubles, plus other less severe long-term effects—were unquestionably worthwhile to him, so once more the result seemed to fully justify the means.
But in the 1980s, most pediatric oncologists still considered stem cell transplants an excessively intensive form of therapy. I had gathered a band of “transplant buddies” from across North America to develop treatment protocols for children with several different forms of cancer we judged incurable with less intensive treatment. Were we right in our judgment? I know today, and in truth I knew back then, that a proportion of these children might have been cured with more conventional chemotherapy—treatment that stopped short of the high intensity that required a stem cell infusion. But the choice of treatment was very much in the hands of the pediatric oncology team at the center where the patient happened to show up. Essentially, it was a straight choice between more aggressive and less aggressive therapy.
Ethical reflections
Healing and harm often walk hand-in-hand together. How much did ego and self-advancement go into the treatment we chose for our patients? Medical research is far from a pristine and selfless entity. A member of our hospital bioethics committee once challenged me about who paid for these experimental and often very expensive treatments. She saw it as highly unethical to charge our patients, which was exactly what we were doing. I had no argument to oppose her view, and shortly afterwards resigned from the ethics committee so I did not have to face such challenging questions.
I remember an interview at that time with the head of the national Pediatric Oncology Group (POG), who discouraged me from studying this ethical issue. I wanted the ethics committee I had recently formed to study whether enrolling patients on POG treatment protocols, which were paid for with federal government funds, was coercive. It certainly felt coercive, in that we rarely if ever explained to the parents of children with newly diagnosed cancer that by enrolling their child on a POG-approved protocol the cost would be met entirely by the government, whereas if the parents chose against enrollment they would have to pay for treatment out of their own pockets. Rather than explain this during our informed consent sessions, it was easier to duck the issue by shielding our families from this stark truth. Money is at the heart of many of the treatment choices parents consent to—whatever that word consent really means.
Soon after that interview, I wrote a poem about this very issue:
Consensus and Consent
Eleven-year-old Kyle’s cancer can still be cured.
At least we believe so, though based on shifting grounds,
its intransigence having stacked the odds against him.
True, more experimental therapies await our testing,
whatever that word experimental has come to mean.
Yesterday’s conference had brought us to consensus,
our new resident quoting from an obscure publication
that highlighted new drugs showing definite promise,
though they were yet to be tested on Kyle.
Kyle, consulted today, says: “No, I want to go home.”
So be it. He has, we allow, reached the age of consent,
whenever that may be. We feel—all in all, taking everything
into consideration—relief that we’ve chanced upon a decision.
It was eleven-year-old Kyle who made his own decision to forgo more experimental treatment. And he had the blessing of his parents, who took him home that very day, shortly to die of his cancer in his own bed. The overall costs of experimental therapies, in terms of lives lost and the attendant suffering of both the children and their families, is beyond measure. But where my shadow once fell on so many young lives, I now see the light of those who survived—children like Ted, grown to adulthood. That is the shadow I now choose to walk beside.
End note
* Ted Haines’ name used with permission.
JOHN GRAHAM-POLE, MD, MRCP-UK, a graduate of University of London, was a clinician and researcher in childhood cancer and palliative care for forty years. He co-directed bone marrow transplant units at Case Western University and University of Florida, co-founded University of Florida’s Center for Arts in Medicine (www.arts.ufl.edu/) and HARP: The People’s Press (www.tryhealingarts.ca), dedicated to the arts and health. He has written thirteen books of fiction, poetry, and non-fiction.
