James Marcum
Waco, Texas, United States

“To form a right Judgment of Diseases, is a very difficult Matter.” With this opening sentence, Giorgio Baglivi (Figure 1) began his 1696 treatise De Praxi Medica, which was translated in 1704 as The Practice of Physick (Figure 2).1 Throughout the treatise, he frames the problems plaguing late seventeenth and early eighteenth-century medicine and proposes their solutions.
Baglivi was born in Croatia on 8 September 1668 as Duro Armeno but was orphaned two years later and raised by an uncle.2 At age fifteen, he was adopted by Pietro Angelo Baglivi, a prominent physician in Lecce, Italy, and given the name Giorgio Baglivi. He was apprenticed to his adoptive father and studied medicine at Naples. In 1691 he moved to Bologna and studied with Marcello Malpighi, eventually becoming Malpighi’s assistant and following him to Rome the next year. In 1696 Baglivi was appointed professor of medicine and anatomy at the Sapienza University of Rome and published De Praxi Medica. He died from malaria in Rome on 15 June 1707 at age thirty-eight.
Baglivi’s aim in The Practice of Physick is stipulated in the book’s subtitle: “Reduc’d to the Ancient Way of Observations: Containing a Just Parallel between the Wisdom and Experience of the Ancients, and the Hypothesis’s of Modern Physicians.” He wanted to embed the theoretical medicine of his day on a foundation of ancient practical medicine, especially the teachings of the Greeks and Hippocrates. Baglivi credited the “Prince of Physicians” for transforming medicine from a discipline founded on opinion and superstition to one based on observation and reason—the two chief pillars for the practice of medicine. But later physicians, especially those from Arabia, separated these pillars into two distinct sects. The first was the “Empirick Sect, which exploding all Theory, and disclaiming all manner of Reasoning . . . trusted to Experience alone in the Cure of Diseases.”3 The second was the “Sect of Rational Physicians,” who, Baglivi claimed, gave “the greatest deference . . . to Reason; partly, because they were afraid of stumbling on the Errors they had charg’d upon the Empiricks.”4 Hence a crisis in medicine arose in which it became “despised in many places,” as he admitted in the preface.
To resolve the crisis and to regain medicine’s once ennobled status, Baglivi endeavored to reposition medicine once again squarely on its two pillars, observation and reason. To that end, he chided the two sects accordingly:

Those who oppose Reason to Experience, whether Empiricks or Rational Physicians, seem to me to be all Mad: For how can we make Reason to act all the Parts of Science, that, as all wise Men ought to acknowledge, is acquir’d by Tryal and Use continu’d thro’ a long progress of Time? And on the other hand, why should Experience be only regarded, and Reason turn’d out of doors? . . . I understand that Queen Reason, that is plac’d above all the rest, by which a Physician looks into the Principles and Causes of Diseases, foretells their progress.5
For Baglivi, both reason and experience or observation were critical for the robust practice of medicine. But the issue arose as to how best to combine them to benefit one another mutually, and Baglivi proposed two ways of doing this.
The first way was to yoke reason to observation. “Observation is the Thread,” he wrote, “to which Reason must point.”6 In other words, reason must be guided or directed by observation or experience. Baglivi’s fear was that the rational physician might not accurately perceive the cause of a patient’s illness unless symptoms were observed at “the sick Man’s Bed.”7 He went on to note that “the Narratives of sick people” are equally critical for practicing attentive medicine. Baglivi named this thorough observation of the patient, which harkened back to Hippocratic medicine, Medicina Prima.
The second way was to yoke experience or observation to reason. “Experience,” noted Baglivi, “likewise unconducted by Reason is often-times fallacious.”8 Experience or observation, unless subjected to critical reason, can be misconstrued or misinterpreted. Baglivi’s fear was that without critical reasoning, an empirical physician might misjudge a patient’s symptoms and make a faulty clinical judgment. For Baglivi, reason involved the theoretical, especially new theories associated with the iatromechanical and iatrochemical schools.9 He named this medicine, which is dependent on science, Medicina Secunda. Thus, the genuine medical practitioner first makes a thorough examination of the patient, gathering sufficient information, and then renders an accurate diagnosis and prescribes an effective therapeutic plan based on the best current medical theories.
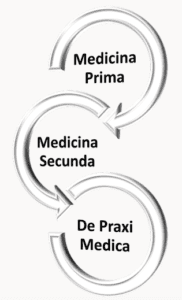
Figure 3. The relationship between Medicina Prima and Secunda for De Praxi Medica (see text for details). Artwork by James A. Marcum on January 20, 2021.
Baglivi identified four steps required to practice medicine effectively vis-à-vis Medicina Prima and Secunda. The first involves making accurate observations of symptoms and chronicling the patient’s narrative, but also noting the season, location, and therapeutic outcomes. The physician is to proceed as “a faithful Scribe” and not to embellish observations with personal opinion, speculation, or vain erudition. The next step is to categorize observations with respect to diagnosis, prognosis, cause, and therapeutic outcomes, among other categories. “Observations are like the Letters of the Alphabet, useless indeed in themselves; but when variously joyn’d, mutually collated and rang’d in order,” according to Baglivi, “they make up the true Idiom of Nature.”10 Once clinical observations are assembled, the third step is what he called “the Method of Digestion,” in which the physician cogitates the intelligibility of various observations. And in the final step, the physician makes a judgment concerning appropriate “general Precepts, comprehending the sum and quintessence of the Art.”11
These general precepts are the aphorisms that serve as guideposts for directing the physician in “true Practice.”12 An important criterion for the aphorisms is that they must be “commensurable” to the particular observations upon which they were formulated: “We must take care above all, that the Mind be directed by Prudence to have the Particulars always in view, and not be left to itself, as being apt in its own Nature to soar to abstracted things.”13 This guided Hippocrates, he claimed, and so must also guide physicians throughout the ages. Baglivi’s practice of medicine, then, was initiated through observations made while attending to and treating the patient, i.e., Medicina Prima (Figure 3). Those observations are the primary support, in conjunction with critical reasoning, that ground the physician’s use of current medical theory to treat the patient, i.e., Medicina Secunda (Figure 3). But Baglivi insisted that the entire process of medical practice—De Praxi Medica—must be prudent in the sense that the physician always focuses diligently on the patient and strives to practice medicine upon both observation and reason for the patient’s benefit.
Baglivi’s practice is relevant for today’s data-driven medicine. Assembling large data-sets of patients and populations enable healthcare professionals to model disease processes and discover novel therapeutics without engaging in traditional hypothesis-driven science. “Data-driven medicine,” argue proponents, “will enable the discovery of new treatment options based on the multi-model molecular measurements on patients and learning from the trends hidden among the diagnoses, prescriptions, and discharge summaries of millions of patient encounters logged by clinical practitioners.”14 Although much progress has been made towards realizing this promise, challenges still remain.15 One challenge is applying such large data-sets effectively to both patients and populations. “For all the talk about the growing mountains of health data,” reports Éanna Kelly, “public health specialists say they are hardly any wiser about how they can apply it to improve overall population health.”16 Baglivi’s advice for this challenge would be to engage in data collection through the “light” of a rational method.17 In other words, reason and observation together are the foundations or pillars for advancing medical knowledge and its practice.
End notes
- Geo. Baglivi, The Practice of Physick (London: Andr. Bell, et al., 1704).
- George Dunea, “Giorgio Baglivi, A Leading Physician of His Time,” Hektoen International: A Journal of Medical Humanities Summer (2018), https://hekint.org/2018/08/30/giorgio-baglivi-a-leading-physician-of-his-time/. W. Bruce Fye, “Giorgio Baglivi,” Clinical Cardiology 25, no. 10 (2002): 487-489. Frederick Stenn, “Giorgio Baglivi,” Annals of Medical History 3, (1941): 183-194.
- Baglivi, The Practice of Physick, 133-134.
- Baglivi, The Practice of Physick, 134
- Baglivi, The Practice of Physick, 7-8.
- Baglivi, The Practice of Physick, 9.
- Baglivi, The Practice of Physick, 206.
- Baglivi, The Practice of Physick, 10.
- James Moores Ball, “The Iatro-Mechanical School: Baglivi, 1668-1707,” Tri-State Medical Journal 5, no. 11 (1898): 576-578.
- Baglivi, The Practice of Physick, 223.
- Baglivi, The Practice of Physick, 226.
- Baglivi, The Practice of Physick, 226.
- Baglivi, The Practice of Physick, 228-229.
- Nigam H. Shah and Jessica D. Tenenbaum, “The Coming Age of Data-Driven Medicine: Translational Bioinformatics’ Next Frontier,” Journal of American Medical Informatics Association 19, (2012): e2-e4.
- David Gotz and David Borland, “Data-Driven Healthcare: Challenges and Opportunities for Interactive Visualization.” IEEE Computer Graphics and Applications 36, (2016): 90-96.
- Éanna Kelly, “Can Data-Driven Medicine Make Us Healthier?,” Science|Business (18 June 2019): https://sciencebusiness.net/healthy-measures/news/can-data-driven-medicine-make-us-healthier.
- Baglivi, The Practice of Physick, 194.
JAMES A. MARCUM, PhD, is professor of philosophy at Baylor University. He earned doctorates in physiology from the University of Cincinnati Medical College and in philosophy from Boston College. He was a faculty member at Harvard Medical School as a molecular biologist for over a decade before joining Baylor’s philosophy department. His research interests include the philosophy and history of medicine and science. He has published eight books and examples of his articles appear in American Journal of Physiology, Journal of Biological Chemistry, Journal of Clinical Investigations, Journal of the History of Medicine, Synthese, and Theoretical Medicine and Bioethics.
