Kayla Peña
Providence, Rhode Island
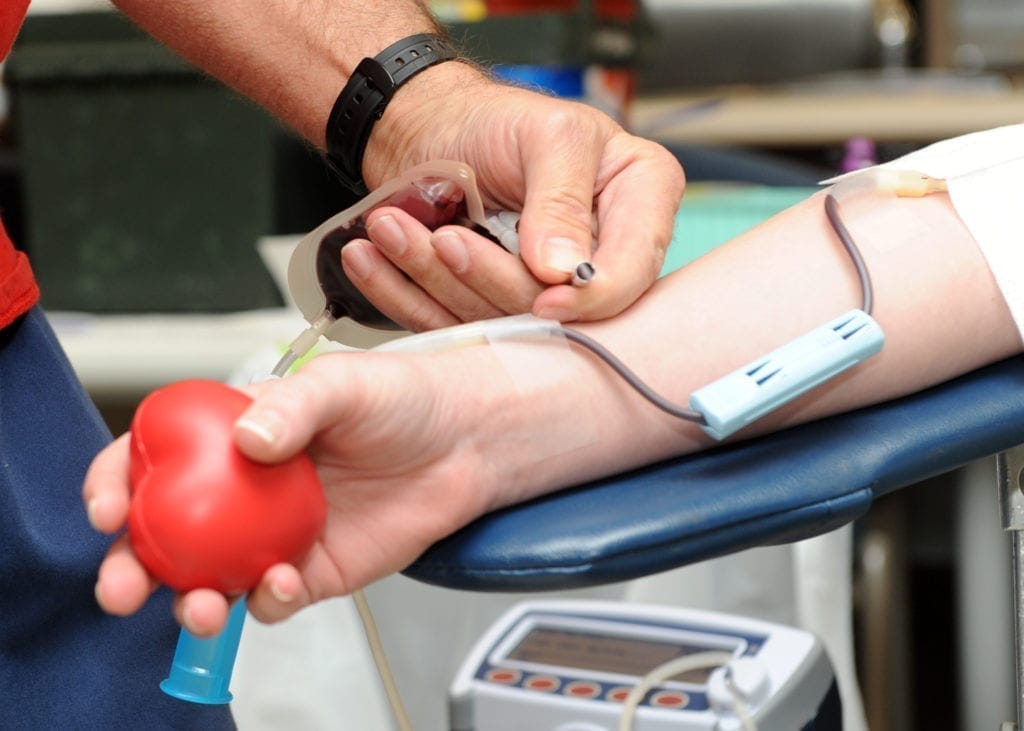
Forty years ago, the University of Michigan and Ohio State University competed in their first “Blood Battle.” Although typically known for their football rivalry, in 1982 the universities decided to expand their competition to see which school could donate more blood.1 Now every November, the students volunteer their veins to help fill donation tubes for the American Red Cross. For every bloodthirsty college student eager to win the competition, there is always at least one pupil who falls victim to the involuntary syncope, anxiety, or even panic attack that accompanies drawing one’s blood.
For years, scientists have tried to understand why individuals have different reactions to blood. While most of the “Blood Battle” participants are unfazed by the sight of blood, 30% of them are expected to faint.2 These students are also more likely to experience panic attacks and become more susceptible to acquiring Blood-Injection-Injury (BII) phobias. A natural uneasiness towards blood becomes a disability when patients begin to refuse vital medical procedures, thus making this condition an important topic.3 When it comes to blood, the competitive college students in the Midwest may help provide an example of why individuals have such different reactions. Understanding the physiology behind vasovagal syncope, the neuroscience underlying fear, and the genetic underpinning of BII phobias will help answer why blood is so distressing to some, while maybe even thrilling to others.
Noah, a freshman student, is terrified of blood, although he does not know it yet. He waits in line with his classmates, excited to participate in his first “Blood Battle” and contribute to the great cause. As Noah approaches the phlebotomist, he sees the needle that will be used to puncture his skin and draw his blood. His brain freezes, his heart starts racing, and before he knows it, he is on the ground, unconscious. Noah has experienced vasovagal syncope. Reflex syncope, a common cause of fainting, begins with a miscommunication between nerves and blood vessels. Specific triggers, such as fear or disgust, create an inappropriate nerve impulse, causing vessel dilation and low blood pressure.4 This combination results in a lack of blood flow to the brain and voilà, Noah faints. All participants are essentially being exposed to the same trigger causing this reaction, however not all students participating in the “Blood Battle” will experience syncope. In attempts to explain this phenomenon, researchers at the University of California Los Angeles (UCLA) showed how subjectively labeling triggers, like blood draws, was an accurate predictor of vasovagal syncope. Participants who labeled their experience as “scary” or “uncomfortable” were more likely to end up like Noah, unconscious and traumatized.5 The clear connection between one’s emotional perception of blood and firing of neurons is not entirely understood; however, scientists believe it can be attributed to the conditioning of the fear sensing areas of the brain: specifically, the amygdala.
The amygdala is called the seat of human emotion. As the body’s “security system,” it warns humans of danger by provoking fear and panic. When people like Noah see or handle blood the activity in this part of their brain significantly increases. Yet in the same way that not all the college students donating their blood will “pass out,” not all of them will experience increased activity in the amygdala. To further understand why these fear-based reactions occur only in a select few, Richard Davidson at the University of Wisconsin sought to outline the subconscious ways humans process fear. After exposing his participants to stimuli such as blood and needles, Davidson used MRI and PET scans to demonstrate a circuit of heightened brain activity between the amygdala and a different area of the brain known as the prefrontal cortex (PFC). The differences in both tonic activation and phasic reactivity in this circuit play a crucial role in governing different reactions to fear.6 In other words, all individuals have neural circuitry that is wired differently, resulting in different responses to fear-evoking stimuli such as blood. This research suggests that students like Noah have negative experiences because their innate fear of blood triggers a miscommunication between the amygdala and the prefrontal cortex.
Unlike the reactive amygdala, the prefrontal cortex is known for being more “pragmatic.” The PFC is the “decision-making” area of the brain where individuals form new ideas. This area of the brain is where people like Noah label blood as a stressor. But what if these individuals, who also seem to easily faint and to have “short-circuited” neural networks, could override their labeled fear by shifting signals in their brain? Like his colleagues at UCLA, Matt Lieberman wanted to show how simply acknowledging stress was able to shift the reactivity from autonomic areas of the brain to more conscious and deliberate ones. In one study, participants who were asked to label emotions displayed on a series of images showed a clear shift from brain activity in their amygdala to their PFC.7 Lieberman’s work suggests that deliberately labeling stress pauses the visceral reaction, allowing for a more enhancing response. These studies suggest that those with a hyperactive amygdala can consciously override their fear of blood by relabeling it as “harmless.” Researchers believe that this classification of stressors is why some may people actually enjoy seeing blood, specifically those who find gore thrilling.8 Although it may take Noah a great deal of conscious effort, by deliberately acknowledging his stress he perhaps will be able to rewire his neural circuits and mitigate his fear of blood.
Understanding the neural networks that influence phobias is important. However, scientists offer that the root of this fear may be buried in our DNA. In the same way cancer can be inherited, familial aggregation of blood injection phobias suggests a genetic component. In 2016 doctors in rural India struggling to provide care for their “blood-phobic” patients started to question whether their fears developed over time or if they were genetically inherited. Starting by identifying the first person in a family lineage with a BII phobia (the proband), Dr. Ab Wani created pedigrees for hundreds of families residing in Aligarh, India. These ancestral records showed that around 61% of the BII phobia cases were such that those suffering had more than one or more first-degree relatives affected by the same disorder. Although similar studies have yet to be replicated in Midwestern college students, the genetic analysis in India suggests that perhaps Noah inherited a Blood-Injection-Injury phobia. Could it be that Noah was destined to fear blood? According to the research, it is not that simple. While the pedigrees in Aligarh did reveal the familial nature of blood phobias, Wani highlighted the significant imprinting effects extreme fear has on the brain. His studies suggest that the careful balance between active genes and environmental influences on neurophysiology impact the propensity towards blood phobia.9
Unlike most medical conditions, blood phobias do not have a clear pathology. This uncertainty may help explain why some individuals are terrorized by the sight of blood, whereas others seemed unbothered or may even enjoy it. The underpinnings of blood phobias provide several theories that may help explain the spectrum of reactions towards blood. Not everyone faints at the sight of blood, but understanding the biological mechanism of vasovagal syncope may help explain how differences in physiology may cause only some to faint. In addition, while not all experience crippling anxiety during a routine blood draw, variations in neural networks provide a neuroscientific outline for the distinction. Scientists have shown this fear may be genetic, suggesting that phobias may be unavoidable.
Yet research also suggests that individuals like Noah have a degree of control over their fear towards blood. Through conscious mental practices like meditation, those suffering from blood phobias can consciously override their involuntary fears. Perhaps Noah is not destined to fall victim to his phobia after all. Perhaps he may be able to use science to overcome his fear and finally win the “Blood Battle.”
End notes
- Slagter, Martin. “Michigan Defeats Ohio State…in Annual Blood Drive.” mlive, December 2, 2019. http://www.mlive.com/news/ann-arbor/2019/12/michigan-defeats-ohio-statein-annual-blood-drive.html.
- Kleinknecht, Ronald A., Robert M. Thorndike, and Marilyn M. Walls. “Factorial Dimensions and Correlates of Blood, Injury, Injection and Related Medical Fears: Cross Validation of the Medical Fear Survey.” Behaviour Research and Therapy 34, no. 4 (April 1996): 323–31. https://doi.org/10.1016/0005-7967(95)00072-0.
- “Blood-Injury Phobia: A Review.” American Journal of Psychiatry 145, no. 10 (1988): 1207–13. https://doi.org/10.1176/ajp.145.10.1207.
- “Vasovagal Syncope.” Cedars Sinai. Accessed December 4, 2019. https://www.cedars-sinai.org/health-library/diseases-and-conditions/v/vasovagal-syncope.html.
- Labus, Jennifer S., et al. “Vasovagal Reactions in Volunteer Blood Donors: Analyzing the Predictive Power of the Medical Fears Survey.” International Journal of Behavioral Medicine, vol. 7, no. 1, Mar. 2000, pp. 62–72., doi:10.1207/s15327558ijbm0701_5.
- Davidson, Richard J. “Anxiety and Affective Style: Role of Prefrontal Cortex and Amygdala.” Biological Psychiatry 51, no. 1 (2002): 68–80. https://doi.org/10.1016/s0006-3223(01)01328-2.
- Lieberman, Matt D. “Putting feelings into words: Affect labeling disrupts amygdala activity to affective stimuli.” Psychological Science 18,(2007) 421-428.
- Carmichael, Sarah Green, Martin E. P. Seligman, Alia Crum, and Thomas Crum. “Stress Can Be a Good Thing If You Know How to Use It .” Essay. In HBR’s 10 Must Reads on Mental Toughness, 71–75. Harvard Business Review Press, 2018.
- Wani, Ab, et al. “Persistence and Inheritance of Blood Injury and Injection Phobia.” Gulhane Medical Journal, 2017, doi:10.5455/gulhane.172838.
KAYLA PEÑA, ScM, MD candidate, is a Clinical Researcher at Brown University. She is a future doctor and active inquirer.
Submitted for the 2019–2020 Blood Writing Contest