Marco Luchetti
Milano, Italy
Introduction
Simulation can be defined as a technique or method to artificially reproduce the conditions of a phenomenon.1 Simulation-based training and education are designed to teach individuals the basic elements of a system by observing the results of actions or decisions through a feedback process generated by the simulation itself. Participants are required to “play” and “act” in the first person in order to manage complex phenomena or relationships in a challenging situation.4 In healthcare, simulation-based education reproducing expert knowledge allows the learner to use hands-on training with simulated clinical scenarios to learn critical thinking and to develop patient care techniques.
Early developments in simulation
At the dawn of aviation, pilots learned to fly on real airplanes: they began as simple passengers, then did a few take-offs, and finally faced a real flight.5 Today, aircraft simulators can accurately reproduce any type of movement and view and find application both in flight and control tower operations. The methodology used to manage flight simulations is known as Crew Resource Management (CRM): a training process based on the resolution of a situation, in which crew members must interact with each other and perform flight operations.6
War simulations inspired so-called business games, i.e. games that introduce a hypothetical company situation, where decisions are made by managing variables in a simulated environment. After the first initiatives in 1956 by the American Management Association (AMA), simulation was introduced in industries, commerce, and universities. Usually, business games involve groups who must make decisions within a corporate setting defined by precise rules.7 In the 1980’s, another technique based on simulation was also developed: the corporate (or organizational) theater.8 This technique, based on the idea of Christian Poissonneau, who invented the so-called “Théâtre d’entreprise,” assumes a learning methodology that uses the techniques of theatrical art to represent different fields of the organization.9
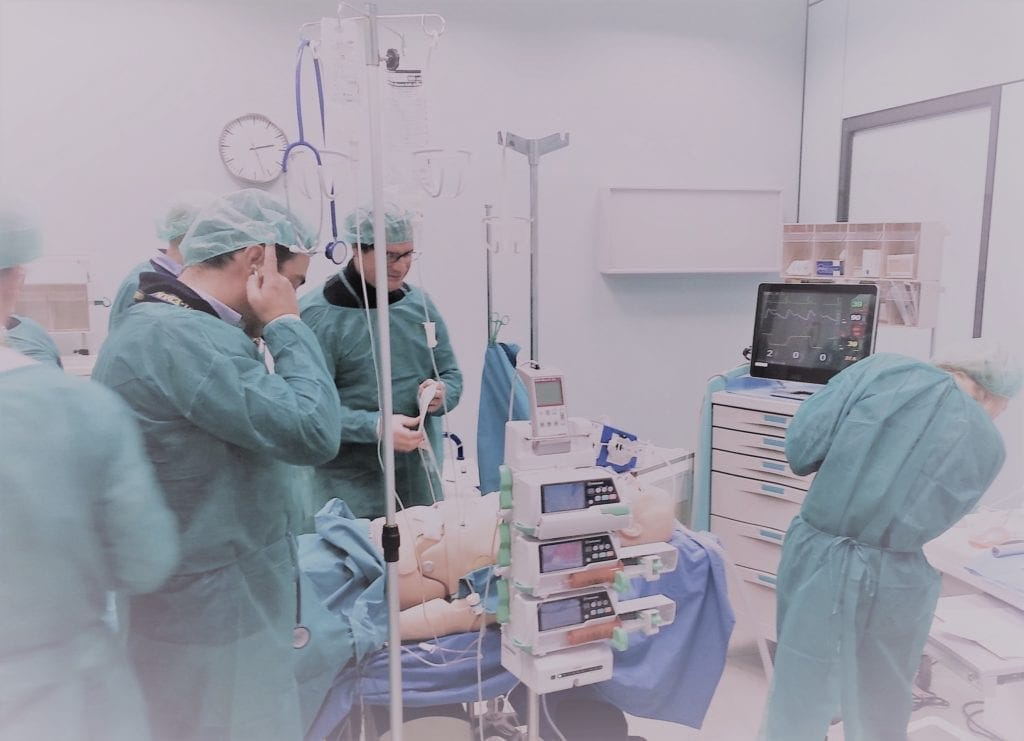
Landing in the healthcare field: Human simulators
Simulation in the field of medicine has spread quite late when compared with aviation and the military. Since ancient times, healthcare professions have exercised theoretical knowledge and skills by practicing on cadavers and animals, and by being gradually exposed to procedures with the help of experts. Recently, however, due to concerns regarding time, patient safety, quality of care, and medico-legal issues, acquiring practical experience this way, especially for novices, is no longer feasible. It is difficult to implement a learning model based solely on experimentation practice.10
In the late 1950’s, Peter Safar showed the advantages of mouth-to-mouth ventilation by decreasing carbon dioxide and increasing oxygenation in patients. While presenting his work, he met a toy manufacturer from Norway named Asmund Laerdal. In the 1960’s they collaborated with anesthesia providers to invent the Resusci-Anne.11 This invention radically changed the way healthcare providers were trained to take care of critically ill patients. Further work resulted in the initiation of chest compressions for use in non-pulsatile patients, so Laerdal added a spring in the chest of the mannequin to train providers in that skill. Resusci-Anne has become a mainstay for educating all healthcare providers and is still used today.12
In the mid 1960’s, when the first simulators were created by Dr. Stephan Abrahamson and Dr. Judson Denson, anesthesiologists began using computer-controlled simulation mannequins.13 SimOne was born: “It breathes; has a heartbeat, temporal and carotid pulse (all synchronized), and blood pressure; opens and closes its mouth; blinks its eyes; and responds to four intravenously administered drugs and two gases (oxygen and nitrous oxide) administered through mask or tube. The physiologic responses to what is done to him are in real time and occur automatically as part of a computer program.” Sim One was clearly ahead of its time: due to the costs of such technology in the early days, few could afford simulation as a teaching tool and its use was almost abandoned. Sim One was never marketed.
In the mid-80’s the environment was better suited for a reintroduction of anesthesia simulators. Two anesthesiologists, David Gaba and Michael Good, revived the use of computer-controlled mannequins and brought about the growth of simulation-based education. In 1986, Comprehensive Anesthesia Simulator Environment (CASE) was a series of simulators being developed by Gaba and DeAnda at Stanford University.14 CASE used commercially available waveform generators to provide signals to actual clinical instruments. Other features included a non-invasive blood pressure cuff, the ability to occlude the left mainstem bronchus, insertion of intravenous lines, CO2 monitoring, mask ventilation, intubation, and auscultation of breath sounds.
At the same time, GAS (Gainesville Anesthesia Simulator) was developed by the team of Good and Gravenstein at the University of Florida.15 The simulator had a palpable pulse, non-invasive blood pressure measurement devices, and a thumb that moved in response to the degree of nerve block and stimulation. GAS was capable of spontaneous ventilation, and monitored O2, N2O, N2, and one volatile anesthetic, which were based on a mathematical model of gas exchange, uptake, and distribution. Good started a simulation company named Medical Technologies Incorporated, or METI.
The benefits of simulation as an educational tool have extended to all stakeholders, increasing the clinical competence of healthcare providers and reassuring administrators that employees are proficient in delivering safe patient care. Learning does not stop at graduation. All healthcare providers must receive continuing education credits to maintain licenses and certifications, and simulation training has been used to teach learners at all levels of experience.
Simulation is a way of consolidating knowledge in a non-threatening manner, so that students can focus on tasks without the worry of harm to the patient. With simulation as a teaching tool, complicated scenarios are repeated until all achieve competence.12 On-site simulation centers facilitate the retention of competent staff and show that an organization is committed to patient safety and the continuing education of employees.
In 1999, the Institute of Medicine published “To Err is Human: Building a Safer Healthcare System,”16 which made evident the prevalence of medical errors resulting in harm to patients. This report shed light on the need for further changes in medical education.17 Simulation has grown rapidly in colleges, universities, and hospitals as a method to offer continuing education to staff. With more students and fewer supervised clinical sites, simulation is a good alternative to patient care that engages students and fosters real life critical thinking and decision making.12 National and international societies now promote and study simulation, such as the Society for Simulation in Healthcare (SSH), the Society in Europe for Simulation Applied to Medicine (SESAM), and the UK National Association of Medical Simulators. International journals such as Simulation in Healthcare and Clinical Simulation in Nursing have also continued to move the field forward.18
Simulation-based education creates a protected environment in which it is possible to learn and teach using errors as resources for action. It involves sensory perception, but at the same time should protect participants from fear related to the possible penalty for mistakes. These characteristics have ensured the success of simulation as a useful and well-established technique for teaching trainees as well as established professionals that require continuing education.4
One of the most important parts of the simulation experience is the debriefing that follows the hands-on clinical use of the mannequin. After a scenario is run, students gather, and a facilitator discusses the strengths and weaknesses of the team. This is where the real learning takes place. Students gain insight into their mistakes and learn from them by reviewing how to handle similar situations differently. In some of the more sophisticated simulation labs, a video is made of the training and brought into the debriefing so everyone involved can see what took place and can evaluate all roles.
Today, it is recognized that healthcare professionals need practice in order to learn new skills and maintain existing ones.19 Simulation-based education, reproducing expert knowledge, allows the learner to use hands-on training with simulated clinical scenarios to learn critical thinking and to develop patient care techniques. The acquisition of higher performance in medicine is directly related to the time spent practicing and receiving feedback during medical training, as well as ongoing learning for medical professionals.
References
- Alessi SM, Trollip SR. Computer-Based Instruction: Methods and Development. Englewood Cliffs, NJ: Prentice Hall; 1991.
- Reigeluth C, Schwartz E. An Instructional Theory for the Design of Computer-Based Simulations. Journal of Computer-Based Instruction. 1989;16(1): 1-10.
- Reed ES. James J. Gibson and the Psychology of Perception. New Haven: Yale University Press; 1988.
- Aldrich C. Simulations and the Future of Learning. San Francisco: Pfeiffer; 2004.
- Page RL. Brief history of flight simulation. SimTecT 2000 Proceedings. 2000:11-17.
- Kanki BG, Helmreich RL, Anca J, eds. Crew resource management (2nd edition). San Diego: Academic Press, Elsevier; 2010.
- Wolfe J. A history of business teaching games in English-speaking and post-socialist countries: The origination and diffusion of a management education and development technology. Simulation & Gaming.1993; 24(4): 446-463.
- Clark T, Mangham I. From dramaturgy to theatre as technology: The case of corporate theatre. Journal of Management Studies.2004; 41(1): 37-59.
- Poissonneau C. Théâtreá la carte- L’entreprise mise en scène. Actualité de la formation permanente. 1992; 120: 68-70.
- Dutta S, Krummel TM. Simulation: a New Frontier in Surgical Education. Advances in Surgery. 2006; 40: 249-263.
- Tjomsland N, Baskett P. Resuscitation greats: Åsmund S. Lærdal. Resuscitation. 2002; 53 (2): 115–119.
- Bradley P. The history of simulation in medical education and possible future directions. Medical Education.2006; 40(3): 254-262.
- Abrahamson S, Denson JS, Wolf RM. Effectiveness of a simulator in training anesthesiology residents. Qual Saf Health Care 2004;13(5):395-397.
- Gaba DM, DeAnda A. A comprehensive anesthesia simulation environment: re-creating the operating room for research and training. Anesthesiology.1988; 69(3): 387-394.
- Good ML, Gravenstein JS. Anesthesia Simulators and Training Devices. International Anesthesiology Clinics. 1989; 27(3): 161–166.
- Donaldson MS, Corrigan JM, Kohn LT, eds. To err is human: building a safer health system. Washington (DC): National Academies Press; Vol. 6. 2000.
- Dawson S, Kaufman J. The Imperative for Medical Simulation. Proceedings of the IEEE. 1998; 86(3): 479–83.
- Alinier G. A Typology of Educationally Focused Medical Simulation Tools. Medical Teacher. 2007; 29(8): 243-250.
- Ericsson KA. Deliberate practice and the acquisition and maintenance of expert performance in medicine and related domains. Academic Medicine. 2004; 79(10 Suppl): S70-81.
MARCO LUCHETTI, MD, MSc, CHSE, was born in Napoli, Italy, in 1964. He graduated in Medicine in 1990 and was board certified in Anesthesia and Intensive Care in 1994. He earned a master’s degree in Pain Management in 2010 and was certified as Healthcare Simulation Educator (CHSE) in 2016. He has been working as an Anesthesiologist & Intensivist for more than 20 years. As of 2017, he works as Clinical Manager, Acute Care, Europe, at GE Healthcare. His professional interests include anesthesia, intensive care, emergency medicine, pain management and simulation. He has a record of over 50 peer reviewed papers, two books and several book chapters.
