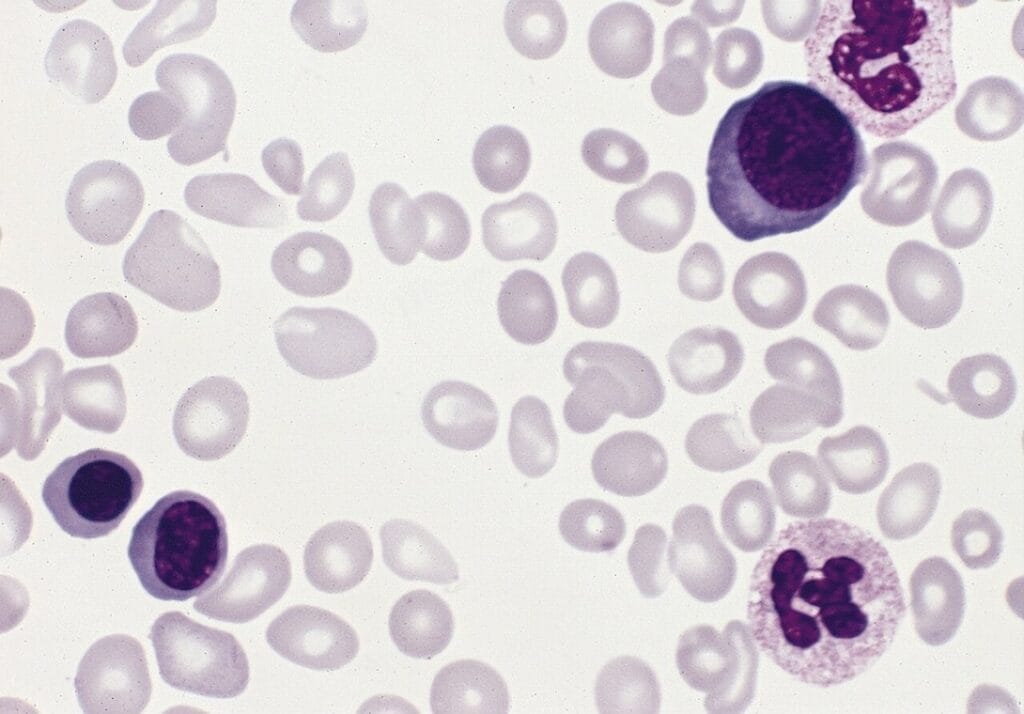
Polycythemia vera is a blood cancer in which the bone marrow generates too many red blood cells. It affects about one in every 50,000 people, primarily men over sixty years old, and is somewhat more common in subjects of Ashkenazi Jewish descent than in other populations. Though classified as a malignant disease, it runs a slowly progressive course, and with modern treatment, those affected have an almost normal life expectancy.
The disease was described in 1892 by the French physician Louis Henri Vaquez, who reported a patient with cyanosis, splenomegaly, and persistent elevation of red blood cells. He recognized that this was a primary disorder of blood production, distinct from cases in which plasma volume is reduced but red blood cell numbers are normal. In 1903, Sir William Osler also wrote about the disease, describing more cases and emphasizing its chronic nature. For some time, the condition was known as the Vaquez-Osler disease.
In 1900, Wilhelm Turk, a Viennese physician, noted that white blood cells and platelets were also elevated in polycythemia vera, suggesting that polycythemia vera was a disorder involving all the cells of the bone marrow. This led to the concept, espoused by William Dameshek in 1953, that polycythemia vera was a member of bone marrow disorders that included essential thrombocythemia and myelofibrosis. This led to the formal designation of criteria for disease and to the eventual introduction of treatments designed to inhibit cellular division and proliferation.
The disease generally has an insidious onset. Some patients have a ruddy or plethoric complexion; others complain of vague symptoms such as headaches, fatigue, or dizziness. Some patients experience intense itching, so-called aquagenic pruritus, often described as a burning or prickling sensation triggered by contact with water, and believed to be due to abnormal histamine release by the proliferating mast cells and basophils. While not dangerous, this symptom of itching can profoundly disrupt quality of life and can be one of the most difficult aspects of the disease to manage.
Another distressing symptom is erythromelalgia: burning pain and redness of the hands and feet caused by platelet-mediated microvascular occlusions. This tends to be characteristic of myeloproliferative neoplasms in general and may respond well to low-dose aspirin. Patients with very high platelet counts are also prone to bleeding episodes, as extremely elevated platelet counts can deplete von Willebrand factor, an essential clotting protein. Its absence has been termed “acquired von Willebrand syndrome.”
The major risk of untreated polycythemia is blood clotting from increased blood viscosity, triggering a heart attack, a stroke, or deep vein thrombosis. The spleen may enlarge and become painful, and some patients may develop peptic ulcers. Often, the disease is discovered as a result of blood work ordered for unrelated reasons. A subset of patients experience transformation into myelofibrosis, a condition in which the bone marrow becomes progressively fibrotic, reducing its ability to produce blood cells. About 2 to 5 percent of patients develop acute myeloid leukemia within 10 years, which has a poor prognosis.
The treatment of polycythemia focuses on managing symptoms, reducing the risk of blood clots, and preventing disease progression. Aspirin twice daily is recommended for most patients to reduce the risk of blood clotting. The oldest and simplest approach is regular venesection, which removes blood from the body, much like donating blood. This reduces the number of circulating red blood cells and is the recommended first-line approach, especially for patients under sixty who have not had any thrombotic complications.
For older patients or those over the age of sixty, hydroxyurea has long been the drug of choice. It was followed in 1998 by the anti-proliferative inhibitor Interferon-alpha, available in new pegylated forms and favored particularly in younger patients and in pregnancy, given its lack of leukemogenic potential.
An important breakthrough came in 2005 when several groups independently discovered a mutation in the Janus kinase 2 (JAK2) gene that leads to constant stimulation of excessive blood cell production. Found in over 95% of patients with polycythemia vera, this mutation is now considered a definite molecular indicator of the disease. It is now possible to confirm the diagnosis using molecular testing rather than relying solely on traditionally accepted clinical and laboratory findings. This discovery enables therapies that block abnormal signaling, control symptoms, shrink the spleen, and enhance quality of life.
The recommended criteria for diagnosing the disease are ever-changing, but, in general, are a hemoglobin level of 18.5 g/dl in men and 18.0g/dl in women. Lower diagnostic levels would require a bone marrow biopsy showing hypercellularity of red blood cells or the demonstration of a JAK2 mutation. It is also helpful to measure erythropoietin levels, which are typically subnormal in contrast to secondary polycythemia caused by severe lung disease or living at high altitudes. New treatments include Rusfertide (approved January 2026 and able to maintain a hematocrit <45% and virtually eliminate the need for phlebotomies), Ropeginterferon alfa-2b (Besremil, increasingly preferred over hydroxyurea for younger patients because it can induce molecular remissions, reducing the JAK2 mutation level), Givinostat, Sapablursen, and Divesiran—all with different mechanisms of action.
Despite the classification of polycythemia vera as a cancer, most patients maintain a good quality of life for years or even decades. The median survival is only slightly shorter than that of the general population, and therapeutic advances are constantly narrowing the gap. It is exciting that, within a period of 20 years, polycythemia vera has gone from a once-untreatable disease to one better understood, shown to be caused by a single molecular mutation, and potentially treatable with an agent specifically developed for it.
