Howard Fischer
Uppsala, Sweden
“Is it even possible, is it logical, is it reasonable for us to treat people who have lost their mind by making them live amongst others who have lost theirs too?”1
– Ugo Cerletti, M.D., 1949
Dr. Ugo Cerletti (1877–1963) trained as a neurologist and had a special interest in the gross and microscopic changes in the brain in neurologic and psychiatric conditions. He was the head of the Neurobiological Institute of the Psychiatric Hospital of Milan from 1919–1924. In 1935 he became chair of the department of mental and neurological diseases at the University of Rome La Sapienza. Cerletti experimented with the possibility of using electric current to produce convulsions in animals.2 The thinking among neurologists at the time was that convulsions could prevent schizophrenia, and that epilepsy and schizophrenia were “antagonistic.” Induced convulsions might be a way, then, of treating schizophrenia.
In the early 1930s, psychiatrist Ladislaus Meduna (1896–1964) produced convulsions in patients with schizophrenia by giving intramuscular injections of various chemical substances. He eventually decided upon pentylenetetrazol, a cardiac and respiratory stimulant that produces convulsions at high doses. This drug, called “Cardiazol” in Europe and “Metrazol” in the US, was dangerous and produced disturbing sensations in patients before the convulsions started.3 At about the same time, Dr. Manfred Sakel (1900–1957), a neurophysiologist and psychiatrist in Vienna, treated patients with schizophrenia with insulin, inducing hypoglycemic convulsions and coma. This, too, was a dangerous procedure. In addition, insulin was extremely expensive.4 This approach, as well as Meduna’s Cardiazol treatments, were stopped after Ugo Cerletti’s introduction of the use of electric currents.
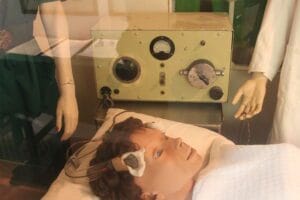
Cerletti’s early experiments with animals involved placing electrodes at both ends of the animal, a “head-to-tail” administration of electric current. This current would pass through the heart, producing arrythmias or cardiac arrest, killing the animal.5 According to legend, Dr. Cerletti observed that in slaughterhouses, cattle would get an electric shock to the head only, which caused the animal to convulse and fall down, making it easier to cut its throat.6 Cerletti and his assistant, Dr. Lucio Bini, tried this technique on hundreds of pigs and dogs and examined their brains in order to detect any possible damage from the electricity or from the seizure it produced. Cerletti was a skilled neuropathologist, and he saw no evidence of damage. The two researchers developed a machine that could safely give electroconvulsive treatment to patients. In 1938, they encountered a man brought in by the police to the hospital, who was delirious and hallucinating. He could not say who he was nor answer any other questions. They gave him a series of eleven convulsion-producing electric shocks, which brought him back to his premorbid state.7
Cerletti and Bini described their results at a conference in Rome and at an international congress in Copenhagen in 1939. Their method was quickly adopted in Europe, being safer, cheaper, and more easily administered than Cardiazol or insulin treatments. It was first used in the US in 1940.8
Electroconvulsive therapy (ECT) is used today for the treatment of severe mental illness that has not responded to other (that is, pharmacologic) treatment.9 The development of psychotropic medications in the 1950s and 1960s made it possible to treat fewer patients with ECT, but ECT is still considered safe and effective. About 100,000 people each year receive ECT in the US.10
Today, a patient receiving ECT receives a general anesthetic and a muscle relaxant. An intravenous line is placed for any medication that might unexpectedly be needed during the treatment. The patient’s blood pressure, heart rate, electrocardiogram, blood oxygenation, electroencephalogram, and electromyogram (measuring muscle activity) are all electronically monitored. The mortality from ECT is about two deaths per 100,000 treatments, mostly from underlying cardiovascular disorders.11
References
- Carlo Patriarca et al. “Ugo Cerletti, Pathologica and electroconvulsive therapy.” Pathologica, 113(6), 2021.
- Stefan Pallanti. “Ugo Cerletti (1877-1963).” American Journal of Psychiatry, April 1, 1999.
- “Pentylentetrazol.” Wikipedia.
- Gianni Faedda et al. “The origins of electroconvulsive therapy: Prof. Bini’s first report on ECT.” Journal of Affective Disorders, 120, 2010.
- Robert Kaplan. “The man who first used ECT: Ugo Cerletti.” Psychiatric Times, May 18, 2021. https://www.psychiatrictimes.com/view/ugo-cerletti.
- “Ugo Cerletti.” Wikipedia.
- Pallanti, “Ugo Cerletti.”
- Antonio Metastasio and David Dodwell. “A translation of ‘L’elettroshock’ by Cerletti & Bini, with an introduction.” Eur J Psychiatr, 27(4), 2013.
- Bruce Wright. “An historical review of ECT.” Jefferson Journal of Psychiatry, 8(2),
- Max Fink. “Electroshock revisited.” American Scientist, 88(2), 2000.
- Emiliano Loria. “A desirable convulsive threshold. Some reflections about electroconvulsive therapy (ECT).” European Journal of Analytic Philosophy, 16(2), 2020.
HOWARD FISCHER, M.D., was a professor of pediatrics at Wayne State University School of Medicine, Detroit, Michigan.
