JMS Pearce
Hull, England

In 1862, Maurice Raynaud (1834–81) of Paris provided one of the finest descriptive accounts in clinical medicine in his doctoral dissertation on episodic digital ischemia. Yet lasting recognition came only after his death. He described twenty-five patients, twenty of whom were female, and with astonishing accuracy deduced the pathophysiology:
In its simplest form, local syncope is a condition perfectly compatible with health… ordinarily females, sometimes without appreciable cause, one or more fingers becomes pale and cold all at once… It is the phenomenon known as ‘dead finger.’ The attack is indolent, the duration varies from a few minutes to many hours. The determining cause is often the impression of cold … sometimes even a simple mental emotion is enough …[T]he attack is followed by a period of reaction, which is often very painful, and which gives place to a sensation quite analogous to that of being numbed by cold …
[I]n more pronounced cases the asphyxial element predominates, pallor is replaced by a cyanotic color… skin had acquired a greater transparence than natural so as to allow subjacent tissues to be perceived; sometimes violet or slate coloured, even becoming black…1
He distinguished the condition from “concussion or compression of a nerve” and noted:
feebleness of the pulse at the commencement… and the patch of white produced by pressure… takes a considerable time before recovering color… which denotes an excessive slowness of the capillary circulation… painful numbness succeeds a sensation of burning and shooting… Meanwhile cutaneous anesthesia is complete and interferes with the prehension of small objects. The period of reaction … irritating tingling sensations… livid patches a vermilion color shows itself at the margin; little by little it gains ground, chasing before it the bronzed color… at the periphery. Finally, a patch of deep red…
These observations led to sections on Diagnosis and The Nature of the Disease in which he clearly recognized its vascular basis:
a sort of painful cramp of the arteries … spasm of vessels irregular or intermittent.
And he noted its origin as a disorder of the “ganglionary system and the great sympathetic nerves of the neck described by M. Claude Bernard.”
Many years later, Sir Thomas Lewis, like Raynaud, concluded that the condition was caused by abnormal susceptibility of the digital cutaneous vasculature to stimulation by cooling, “a local fault.”2 Lewis first distinguished primary Raynaud’s disease from secondary Raynaud’s phenomenon. The secondary, symptomatic form was reported by Alice Hamilton MD (1869–1970), an accomplished pioneer in occupational medicine. She reported “spastic anemia” in 106 out of 123 stonecutters in Indiana with similar symptoms attributable to a rapidly vibrating air hammer used to cut limestone.
Among men who use the air hammer for cutting stone there appears very commonly a disturbance in the circulation of the hands, which consists in spasmodic contraction of the blood vessels of certain fingers, making them blanched, shrunken, and numb. These attacks come on under the influence of cold, and are most marked, not while the man is at work with the hammer, but usually early-in the morning or after work… The condition is undoubtedly caused by the use of the air hammer…3
This became known as hand-arm vibration syndrome or occupational Raynaud’s phenomenon. Raynaud’s phenomenon may be secondary to smoking, vasoconstrictor drugs, hyperviscosity syndromes such as cryoglobulinemia, pulmonary hypertension, or autoimmune disorders such as systemic sclerosis and systemic lupus erythematosus (SLE).
Raynaud advised avoiding cold, wrapping the limb in close-fitting cotton wool, and opium to calm the atrocious pains of mortification of the extremities. Most importantly, despite the title, he stressed the benign nature of primary Raynaud’s disease, noting that “it is not a true gangrene which is produced.” By contrast, secondary Raynaud’s phenomenon can result in ischemic ulcers and gangrene.
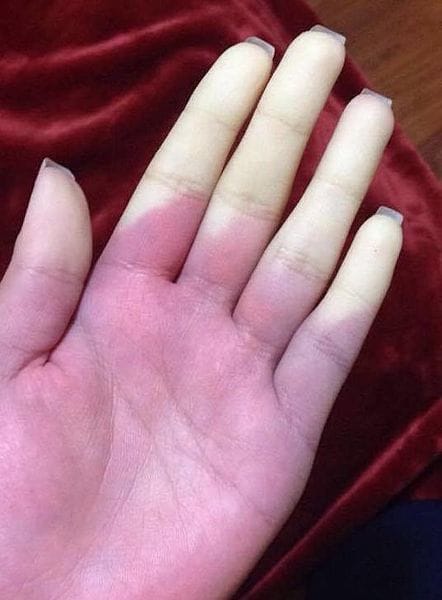
The classical triad comprises pallor caused by vasoconstriction, cyanosis from stagnation of deoxygenated blood, and finally redness from reperfusion.
The prevalence of Raynaud’s phenomenon is approximately 5% of the population. Primary Raynaud’s disease, or idiopathic episodic digital vasospasm, accounts for about 90% of patients with these symptoms.4,5 The onset is usually before the age of forty, more frequently affecting women than men. Cold and emotional stress are common precipitants. The etiology of the episodic vasoconstriction is still uncertain but has been ascribed to dysregulated neuroendothelial control of vascular tone.6 The number of calcitonin gene-related peptide (CGRP) immunoreactive neurons is reduced in the skin of patients, and an increased alpha 2c–adrenergic response has been shown in primary Raynaud’s phenomenon.
Modern investigations demonstrate defects in the vascular and microvascular circulations using infrared thermography, nailfold capillaroscopy, and Doppler ultrasound. Anatomical studies have identified the importance of peptidergic nerves in the control of vascular tone. Vasodilating calcium channel blockers such as nifedipine and amlodipine are the first line of therapy. Alternatives for severe disease include phosphodiesterase-5 inhibitors and intravenous prostaglandin analogues. Cervical sympathectomy is usually unsuccessful. In intractable cases, botulinum toxin A injected into the digital neurovascular bundles of all five digits via a dorsal or palmar approach has been reported to improve pain, ulceration, and perfusion.7
Auguste Gabriel Maurice Raynaud (1834–1881)

Maurice Raynaud was born in Paris, the son of Jacques-Auguste Raynaud, a professor at the Collège Royal Bourbon (Lycée Condorcet) and Félicité-Marie Vernois.8
He studied medicine in Paris, graduating in 1862 with his thesis De l’asphyxie locale et de la gangrène symétrique des extrémités. Few others have found eponymous fame with their thesis. He also obtained the Doctorate of Letters (LLD) with another work: Les Médecins au temps de Molière.
Raynaud applied three times for the Chair of History of Medicine and Surgery, but failed to be appointed, possibly owing to anti-clerical discrimination. He became Médecine des hôpitaux in 1865 and held relatively junior appointments at the Hôtel Dieu, Laboisière, and Hôpital de la Charité.9 He published over fifty clinical papers in the General Archives of Medicine, the Bulletin of the Anatomical Society, and the Weekly Gazette of Medicine and Surgery. He was also a poet, critic, instructor, historian, philosopher, and Catholic standard-bearer. WL Cooke, a physician from California, described him as “an erudite eclectic with a firm grasp of neurophysiology, he was also a pre-Darwinian exponent of evolution with an unashamedly theocentric world view.”10 He published a paper on rabies with Louis Pasteur and several articles on pathology and respiratory diseases.
During the War of 1870, he was in charge of the Relief Society ambulance service and was made an officer of the Légion d’honneur in 1871. He received a gold medal for treating epidemic cholera in 1866 and was elected to the Académie de Médecine in 1879.
Only after Jonathan Hutchinson (1828–913) had called attention to his syndrome was it generally recognized. Hutchinson had described his own cases11 including a patient with “Acro-scleroderma with Raynaud’s phenomena.”12
Aged forty-six, Raynaud died of a heart attack on 29 June 1881 and was buried at the Cimetière du Père Lachaise in Paris.
References
- Raynaud M. De l’asphyxie locale et de la gangrene symmetrique des extremities. Paris: Rignoux, 1862. [On local asphyxia and symmetrical gangrene of the extremities] translated by T. Barlow, London: The New Sydenham Society, 1888, 99-101, 138-40, 143-5, 147-50.
- Lewis T. Experiments relating to the peripheral mechanisms involved in spasmodic arrest of the circulation in the fingers, a variety of Raynaud’s disease. Heart 1929;15:7-101.
- Hamilton A. Effect of the air hammer on the hands of stonecutters. Monthly Review of the U.S. Bureau of Labor Statistics 1918;6(4):25-33.
- Belch JJF. The Phenomenon, Syndrome And Disease Of Maurice Raynaud. Rheumatology 1990;29:162-165.
- Andrews J. Maurice R Raynaud and his Protean Disease. Journal of Medical Biography. 1997;5(1):46-50.
- Kaheleh B, Matucci-Cerinic M. Raynaud’s phenomenon and scleroderma. Dysregulated neuroendothelial control of vascular tone. Arthritis Rheum 1995;38:1-4.
- Dhaliwal K, Griffin M F, Salinas S. et al. Optimisation of botulinum toxin type a treatment for the management of Raynaud’s phenomenon using a dorsal approach: a prospective case series. Clin Rheumatol 38, 3669-76.
- Pearce JMS. Raynaud’s phenomenon. J Neurol Neurosurg Psychiat 1989; 52;594.
- Maurice Raynaud Obituary. Progrès Medical 1881;9:552-3.
- Cooke WL. Maurice Raynaud, Christian Humanist. The Linacre Quarterly 1981;48:117-24.
- Hutchinson J. Raynaud’s phenomenon. Arch Surg 1900;11:330-6.
- Hutchinson J. Two lectures on acropathology, Raynaud’s phenomenon and allied conditions. Med Week/Sem Hôp 1893;85:97.
JMS PEARCE is a retired neurologist and author with a particular interest in the history of medicine and science.
Highlighted in Frontispiece Volume 18, Issue 1 – Winter 2026 and Volume 15, Issue 3 – Summer 2023
