Stanley Gutiontov
Chicago, Illinois, United States
The bad rap
“And the pig, though it has a split hoof completely divided, does not chew the cud; it is unclean for you.”
—Leviticus 11:7

Pig: a word variably defined as “a young domesticated swine not yet sexually mature” or “a dirty, gluttonous, or repulsive person.”1 Pork may harbor within it hundreds of infectious agents, at least two of which have been known since antiquity: the pig tapeworm, Taenia solium, and Trichinella spiralis, the parasite that causes trichinosis. Tapeworms were known to the ancient Egyptians, and T. solium itself was discussed in Aristotle’s History of Animals under the guise of “measled pork”2 even today, neurocysticercosis secondary to T. solium infection is one of the leading causes of seizures and epilepsy in the developing world.3 Figures as famous as Rudolf Virchow participated in research leading to the discovery of the life cycle of T. spiralis4: the “uncleanliness” of the pig has been well documented by some of the greatest thinkers of all time.
The genus Sus has been subjected to this bad rap for nearly the entire span of human history: in 2009, millennia after Aristotle’s description of “measled pork,” the global outbreak of swine flu precipitated hysteria and further vilified the creature. Vigilance is, of course, necessary. Ignorance is not. One must not disregard either of the implications of the similarity between sus scrofa domestica and homo sapiens sapiens: a creature that can serve as an intermediate reservoir of influenza that might later jump to us is also, by the very virtue of its biological proximity, one of the most useful—if not the most useful—animals in the history of medicine.
Inspired vivisection

In the above painting by Dutch Golden Age painter Adriaen van Ostade, pupil of Frans Hals and contemporary of Rembrandt van Rijn, the pig is not a creature of filth; rather, it is all inspiration, warm light, artistic revelation. Moved to change his painterly style by Rembrandt’s superlative skill with light, Ostade completed his masterpiece one year before the older painter’s more famous Der geschlachtete Ochse. Here, the splayed pig is a veritable muse.
So it has been from time immemorial. Galen of Pergamon, the most important figure in classical medical science, used animals in his many dissections: the ox (for brain anatomy), the macaque (for cranial nerve anatomy), and the pig (for vivisection). During one of his experiments, as he was carrying out a strapped-down, struggling, and squealing pig, he accidentally cut its recurrent laryngeal nerves: the pig continued to struggle but now did so noiselessly. Following this serendipitous (the pig would beg to differ, if it could) occurrence, Galen went on to show that cutting both of these nerves in a menagerie of animals eliminated vocalization. His 2nd-century fumble with the pig became the first experimental evidence that the brain controls behavior.
So famous did the squealing pig experiment become that Renaissance editions of Galen’s writings contain frontispieces depicting him cutting these nerves in a pig, Leonardo da Vinci produced a drawing of the recurrent laryngeal nerves, and Andreas Vesalius dedicated a large part of the last chapter of his 1543 opus De Humani Corporis Fabrica to the dissection of live animals, including a vivid image of an about-to-be vivisected pig.5
An aside: the 1923 Nobel Prize in medicine
The Nobel Prize in Physiology or Medicine 1923 was awarded jointly to Frederick Grant Banting and John James Rickard Macleod “for the discovery of insulin.”
—Nobel Prize Announcement, 1923
The pig is—as was clear to both Galen and Vesalius—an anatomist’s marvel: the remarkable degree of similarity between the internal anatomy of the pig and that of the human is uncanny. The story only begins there: in physiology, too, we are astoundingly alike. On January 23, 1922, Leonard Thompson, a 14-year-old boy who lay dying of diabetic ketoacidosis at Toronto General Hospital was given the first injection of purified insulin; his symptoms completely reversed.6 Though Banting, Best, and Macleod first performed this miracle using hormone isolated from dog pancreas, the mass production of insulin until 1980—and therefore life-saving treatment for millions of people worldwide—required the pancreas of the ox or the pig. While the former yields insulin that differs from human insulin by three amino acids, pig insulin is just one amino acid shy of the real thing: a truly phenomenal molecular likeness.
Hand on your heart
Big man, pig man, ha ha, charade you are
You well heeled big wheel, ha ha, charade you are
And when your hand is on your heart
You’re nearly a good laugh
—Pink Floyd, Pigs (Three Different Ones)
While the pharmaceutical factories were busy churning out purified pig insulin, the saga of the pig in medicine swung from molecular biology back to anatomy. A 1964 news bulletin in the Journal of the American Medical Association reads “pigskin dressings and immediate excision were both advocated for the treatment of burns at the 49th Clinical Congress of the American College of Surgeons . . . ”7 Evidence is then presented supporting the clinical benefit of such xenotransplantation—the transplantation of cells, tissues, or organs from an individual of one species into an individual of another. The burn wounds healed faster, experienced fewer infections, and the transplants fell away of their own accord in a few weeks’ time without noxious effects. These first successes with xenotransplantation were occurring at an immensely opportune time: it was in the 1960s that the first evidence supporting immunologic rejection came to light.
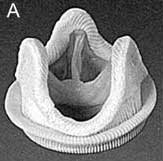
Just a decade after the results with pigskin and burn treatment in humans, a group of French surgeons led by Alain Carpentier—now the head of the French Academy of Sciences—delved into another anatomic realm by performing the first successful heart valve replacement surgery using a xenograft.8 If the use of pigskin in burn treatment seems a small novelty, heart valve replacement is most assuredly not. By 1976, the first commercially available biologic heart valve (Medtronic’s Hancock porcine valve) was introduced. Today, more than 100,000 people in the U.S. with severe heart valve dysfunction need valve replacement surgery and many of them receive bioprosthetic valves from that most unlikely of creatures: the pig.9
Chimera
The creatures outside looked from pig to man, and from man to pig, and from pig to man again; but already it was impossible to say which was which.
—George Orwell, Animal Farm

While the Kafkaesque metamorphosis described in Animal Farm is the stuff of fiction, there are now millions of people walking around with pig parts sewn to one of their vital organs. If this alone is not sufficiently astounding, consider this: valves may very likely be just the beginning.
In the early 2000s, several research groups took the first steps in surmounting the immunologic hurdles first discovered in the 1960s. Using transgenic techniques, scientists succeeded in knocking out the pig alpha-1,3-galactosyltransferase gene that is responsible for some of the immunologic rejection seen in transplantation.10Thomas Starzl, considered by many to be the father of modern transplantation, said the following in regard to such techniques: “Cloning . . . has been done by nuclear transfer. . . . That is what I think may allow enough alteration in pig organs to make them comparable to allografts [organs from humans].”11 If this is indeed the case, then along the Blue Ridge Mountains in Vermont, a company named Revivicor owns a farm that will determine the future of transplantation medicine. On that farm, frolicking with hundreds of other pigs are several transgenic pigs marked only by their slightly punched out ears. With them, Revivicor hopes to accomplish its self-stated goals: the replacement of pancreatic islets in order to cure type 1 diabetes and the production of pig hearts and kidneys for long-term transplantation as well as pig livers as bridges to definitive transplantation.12
These fantastical chimeras, rivaling the fabled sphinx, are just the tip of the iceberg: similar genetic techniques have produced pigs that are excellent models for research in cystic fibrosis, cardiovascular disease, and Alzheimer’s. Perhaps George Orwell was correct on more accounts than one: by better understanding pigs, we will learn to better understand ourselves.
Galen could not have imagined that the relatives of that mute pig, struggling against its inevitable vivisection, would transform medicine. From his initial demonstration of the connection between the brain and behavior to the million-dollar transgenic pigs in Vermont, the admirable pig has evolved uses consistently outpacing our knowledge. Pig is no longer an expletive; on the contrary, we should be honored to be called pig men: artificial skin, valves, and all.
References
- “Pig.” Merriam-Webster Dictionary. © 2012 Merriam-Webster Dictionary Incorporated, [cited 2013 25 Feb] http://www.merriam-webster.com/dictionary/pig.
- Wadia, N., Singh, G., Taenia Solium: A Historical Note in Taenia Solium Cysticercosis: From Basic to Clinical Science 2002, CABI Publishing
p. 157-168. - DeGiorgio, C.M., et al., Neurocysticercosis.Epilepsy Curr, 2004. 4(3): p. 107-11.
- Blumer, G., Some remarks on the early history of Trichinosis (1822-1866). Yale Journal of Biology and Medicine 1939(6): p. 581-588.
- Gross, C.G., Galen and the Sqealing Pig, in The Neuroscientist, 1988. p. 216-221.
- The Nobel Prize in Physiology or Medicine 1923. [cited 2013 25 Feb]; Available from: http://www.nobelprize.org/nobel_prizes/medicine/laureates/1923/
- Pigskin Grafts, Excision for Burns. JAMA, 1964(3): p. 35.
- Carpentier, A., From Valvular Xenograft to Valvular Bioprosthesis: 1965—1970. Ann Thorac Surg, 1989. 48: p. 73-74.
- Vesely, I., Heart Valve Tissue Engineering. Circulation Research, 2005. 97: p. 743-755.
- Platt, J.L., Knocking out xenograft rejection. Nat Biotechnol, 2002. 20(3): p. 231-2.
- Revivicor: Curing human disease through regenerative medicine. 2010; Available from: http://www.revivicor.com/about.html.
- Whyte, J.J. and R.S. Prather, Genetic modifications of pigs for medicine and agriculture. Mol Reprod Dev, 2011. 78(10-11): p. 879-91.
STANLEY GUTIONTOV is a third-year medical student at Feinberg School of Medicine in Chicago. He enjoys writing short stories and performing slam poetry, studying history and literature, and getting people excited about learning. He hopes to one day work in oncology.
Highlighted in Frontispiece Volume 5, Issue 3 – Summer 2013
