JTH Connor
St. John’s, Newfoundland
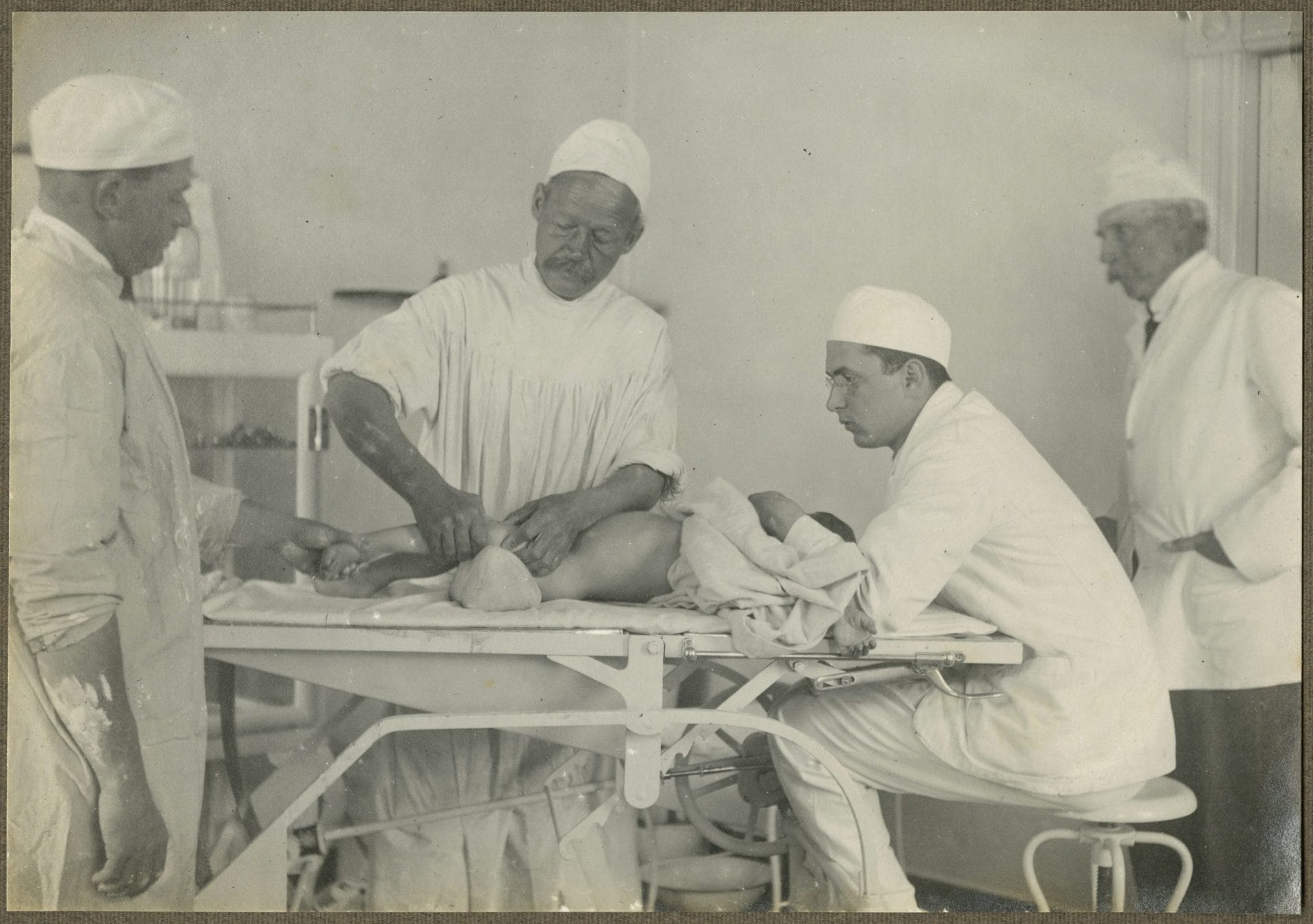
In his own time Sir Wilfred T. Grenfell (1865-1940) was a legend for his inspirational role among the fisher families of coastal Labrador and Newfoundland, a remote region in the North Atlantic that became a Canadian province only in 1949. Between the time of his arrival in 1892 until his death, this English doctor created a network of hospitals, hospital ships, nursing stations, schools, orphanages, and co-operative stores in the most remote zones of this oldest of British colonies. This independent healthcare system was funded largely through charitable donations from people in Canada and Britain, but mostly from those in the United States. His charismatic lectures delivered routinely at Ivy League universities and church assemblies further resulted in a steady stream of highly qualified young men and women who volunteered their labor for his cause. Many well-established American and British physicians and nurses also traveled to the far north to offer their services gratis, while availing themselves of the opportunity to reinvigorate their own bodies and souls. By the 1930s Grenfell’s name was a household word in most middle-class and elite homes, especially in the northeastern United States. As physician, missionary, and humanitarian, Grenfell received many eponymous tributes–streets, schools, a college, a museum, a regional health authority, and a coast guard vessel. His most vaunted tribute may be the medical-themed stained glass triptych in the National Cathedral of Washington, DC, in which Christ the Healer occupies the central lancet window flanked by Louis Pasteur on his right and Wilfred Grenfell in parka and full winter gear on his left.1
Biographical accounts2 and his autobiographical writings3 attest to Grenfell’s strong professional skills as health advocate, scholar, leader, professional, communicator, and collaborator—roles identified as required core medical competencies within the current Canadian Medical Education Directives for Specialists framework (CanMEDS), now the gold standard for medical faculties across Canada and which have been adopted and adapted in countries such as Australia, New Zealand, Germany, Switzerland, and Denmark.4 In 1997 he was inducted into the Canadian Medical Hall of Fame under the category of health leadership.5 But how did he fare as clinician and the key CanMEDS role of medical expert? Although a photograph on the jacket cover of the most scholarly and authoritative biography of Grenfell shows him in a short white coat attending a patient, we know little about his life and career as a physician at the bedside.
Recent research, however, allows us to address Grenfell’s clinical skills. One element of a larger medical history project6 has been the digital preservation and indexing of almost all clinical admission case-books from 1904 to 1940 of the major hospital of the International Grenfell Association (IGA—founded in 1914) in St. Anthony at the tip of Newfoundland’s northern peninsula. This hospital was home base for Grenfell. The approximately 15,000 redacted files provide a searchable electronic database of information about health care workers (physicians and nurses), diagnoses, treatments, patients (age, sex, place of origin, religion, occupation, but not their names or other unique identifiers), and other information such as mode of travel to hospital (dog sled/komatik, schooner, mail steamer, or small boat). Analysis of the 6,185 extant hospital admission case-book records for 1904 to 1930 show that Grenfell was either the primary or secondary physician for 216 patients, who hailed from all districts across the island and the southern Labrador coast. Two-thirds of these patients were adults, over half were men, and most (73%) were surgical cases. A good or satisfactory outcome was reported in 69%; 13% were deemed to be bad or marginal outcomes, or deceased; the remainder were unspecified. Average hospital stay was thirty-nine days.
As a doctor in the major hospital serving the population of a vast region, Grenfell treated a wide range of injuries, ailments, and conditions: occupational accidents such as gunshot wounds, severed toes, hatchet cuts, and leg fractures; routine cases of inguinal hernia, hemorrhoids, varicose veins, appendicitis, tonsillitis, and septicemia; congenital club feet and other orthopedic deformities; cancerous tumors; infectious diseases such as measles, poliomyelitis, and, in 1918, Spanish influenza. But by far the most common condition was tuberculosis, in almost all its debilitating forms: pulmonary, spinal and vertebral (Pott’s disease), testicular, glandular, and of the joints (hip, knee, and shoulder).
Taxing cases illustrate Grenfell’s faith in his own skills. In December 1909, a thirty-two year-old fisherman was admitted to hospital with Jacksonian epilepsy. Grenfell undertook a rigorous patient history, then wrote to the prominent neurosurgeon Harvey Cushing at Baltimore’s Johns Hopkins University. Cushing’s reply of February 1910 gave an assessment of the case; soon after “acting on advice from Dr. Cushing,” Grenfell trepanned the patient’s skull, creating a hole of about 1¾ inches in diameter to facilitate decompression. On May 9, 1910, the patient returned home “feeling very well.” Later that year this man returned to St. Anthony where he underwent a similar but smaller operation; in 1912 he was reported to be in general good health with fewer and less severe convulsions, but suffering occasional episodes of aphasia. While trepanation was not exceptional at that time, the chutzpah demonstrated by Grenfell in contacting Cushing was remarkable.
Although Grenfell’s hospital life (which would also have included Out-Patient Department duties) was less arduous than those of his colleagues who bore the brunt of the IGA medical and surgical workload, his clinical activities and role as “medical expert” ought not to be underestimated. While limited, Grenfell’s duties at the St. Anthony hospital allowed him to keep his hand in as a doctor, much as busy deans of medicine who may continue with an occasional clinic in addition to their administrative duties. More importantly, Grenfell was active as a physician on board the IGA’s several hospital ships, visiting remote communities along the southern Labrador coast during the summers when thousands of fishers and their families migrated to those regions, along with permanent coastal residents. A useful insight to Grenfell’s clinical skills is found in letters sent from patients that were frequently published in the mission’s monthly magazine Among the Deep Sea Fishers. They attest to Grenfell’s caring attention while these men, women, and children were in hospital in St. Anthony, along with his practice of following up upon their return to their far-flung homes.
As Grenfell’s biographer Ronald Rompkey aptly noted, “For people growing up in Newfoundland and Labrador in the latter half of this [twentieth] century, the life of Wilfred Grenfell presents ambiguities.”7 Clearly Sir Wilfred Grenfell was a well-rounded doctor and an excellent role model. But he could be paternalistic to women nursing staff8 — a trait not unusual among doctors in a previous era. Also St. Anthony hospital personnel in the late 1920s under Grenfell’s authority flirted with the discredited science of eugenics and the surgical sterilization of young women deemed to be mentally deficient.9 It is also known that young children in the orphanage and mission school in St. Anthony were selected to participate in nutrition experiments in the 1930s, a use of research subjects that currently would not pass muster.10 Recently, the issue the maltreatment of children in IGA orphanages has emerged.11 But these were different times with different standards of conduct, which is why back writing the present on to the past, if it is to be done at all, ought to be done judiciously. Yet even in the post-colonial world when Grenfell’s star has mostly faded, his name and legend still retain some cachet for their inspirational value in medical literary circles.12
References
- E.R.Crimi and D. Ney, Jewels of Light: The Stained Glass of Washington National Cathedral (Washington, DC: Washington National Cathedral Guidebooks, 2004).
- R. Rompkey, Grenfell of Labrador: A Biography (Montreal: McGill-Queen’s University Press, 2009).
- W.T. Grenfell, Forty Years for Labrador (New York: Houghton Mifflin Company, 1932).
- J. R. Frank and D. Danoff, “The CanMEDS Initiative: Implementing an Outcomes-based Framework of Physician Competencies,” Medical Teacher 29 (2007): 642-47.
- http://cdnmedhall.org/inductees/sir-wilfred-grenfell
- J.T.H.Connor, J.J. Connor,M.G. Kidd, and M. Mathews, “Conceptualizing Health Care in Rural and Remote Pre-confederation Newfoundland as Ecosystem,” Newfoundland and Labrador Studies30 (2015): 113-38.
- Rompkey, Grenfell of Labrador, p. ix.
- H. Coombes-Thorne, “Conflict and Resistance to Paternalism: Nursing with the Grenfell Mission Stations in Newfoundland and Labrador, 1939-81,”inM. Rutherdale, (ed.),Caregiving on the Periphery: Historical Perspectives on Nursing and Midwifery in Canada(Montreal: McGill-Queen’s University Press, 2010) p. 210-42.
- J.T.H. Connor, “The ‘Human Subject,’ ‘Vulnerable Populations,’ and Medical History: The Problem of Presentism and the Discourse of Bioethics,” Canadian Bulletin of Medical History(forthcoming 2016).
- D. Steven and G. Wald, “Vitamin Deficiency: A Field Study in Newfoundland and Labrador,” Journal of Nutrition(21) 1941: 461-7.
- See http://www.cbc.ca/news/canada/newfoundland-labrador/residential-school-students-still-want-apology-compensation-1.3245841 and http://www.cbc.ca/news/canada/newfoundland-labrador/judge-approves-residential-school-settlement-1.3782105
- J.T.H. Connor, “Putting the ‘Grenfell Effect’ in its Place: Medical Tales and Autobiographical Narratives in Twentieth-Century Newfoundland and Labrador,” Papers of the Bibliographic Society of Canada, 48 (2010): 77-118.
JTH CONNOR is the John Clinch Professor of Medical Humanities and Professor of History, Faculty of Humanities and Social Sciences at Memorial University of Newfoundland. He was senior editor of the Canadian Bulletin of Medical History and is currently co-editor of the McGill-Queen’s University Press Studies in the History of Health, Medicine and Society series. He has written widely on the history of medicine in 19th– and 20th-century North America and other topics.
Acknowledgements
The assistance of John R. Matchim who retrieved and compiled information from the hospital admission casebooks file database is gratefully acknowledged. This project was funded in part through CIHR Grant HOM 98740.

One response
My grandmother was his nurse at one time. Her stories were awesome.