Jessie Seiler
Israel
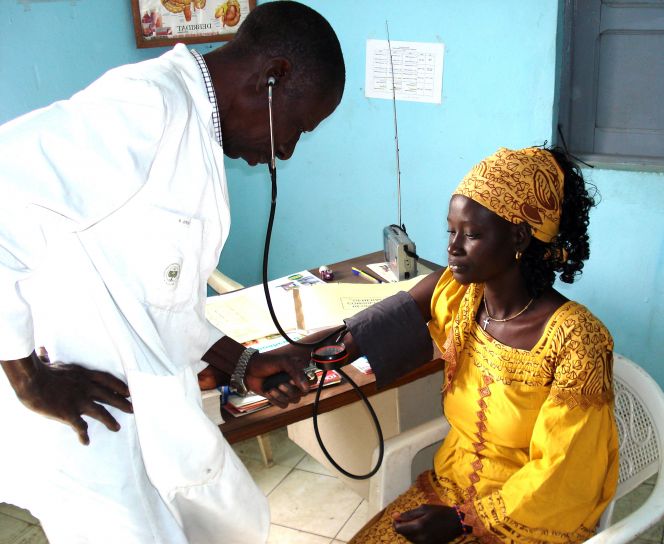 |
| Health clinic in Senegal |
Before beginning my medical education, I spent two years as a health education Peace Corps Volunteer in a small village in the middle of Senegal, in West Africa. When I used to visit Ndiago’s health post, a miracle staffed by able and educated men and women, I usually spent some time in the waiting room. Three tiled benches built out of the walls line three sides of the room; doors lead outside and into the doctor’s office, a few examining rooms, and a well-stocked, carefully organized pharmacy. For an American traveling abroad who might be forced by accident or illness to look for medical help in an extremely remote corner of the world, this scrupulously clean, bustling place would have been a reassuring sight. But the employees at this health post are responsible for an area covering around twenty villages, many of which are far away enough to be tough trips for the seriously ill. Despite this difficulty and the reluctance to make the trip, the waiting room is often packed by mid-morning. After all, there are not a whole lot of doctors and nurses to go around in rural Senegal.
Ndiago is a small village, and it is pretty far off the beaten track of the national highway. Most people come and go by horse-drawn carts. So the village might not immediately strike the mind as a place where two worlds meet and try to become comfortable with one another. When I lived there, I was constantly noticing little bits of my world being easily assimilated into Senegalese daily life. I was the only one who thought that “Houston” brand cigarettes in red and white Marlboro-esque packages were funny. Girls wear traditional printed skirts and ragged t-shirts with HOLLYWOOD emblazoned across the chest in silver sequins without a trace of awareness. Almost every public transit auto sports colorful stickers of Madonna’s face, Barack Obama’s name, and the Mercedes logo. And all of this with no sense of absurdity, no interest in the ideas behind the images, and no discomfort at all.
But one place where I initially assumed that such collisions between two cultures would sit less easily on the Senegalese soul was this waiting room. The idea of a waiting room itself does not translate too readily. In the United States, when you want to see your doctor, you call up and make an appointment. The waiting room is where you get stuck if you are early, or if your doctor is running a bit behind schedule. The first untranslatable concept in this waiting room in Ndiago, then, is time. Ndiago has about 275 people, and, out of those, perhaps ten of could be absolutely depended upon at any point to know exactly what the time is or the exact day of the month or week. When I lived there, someone would occasionally ask me what day of the “white person month” it was (for example, the 31st of October), but I rarely saw that information put to any use. Time, for most people in the village, is figured differently. The call to prayer comes five times a day. If you want to leave the village, you catch a horse cart between sun-up and the beginning of the hot part of the day, or you wait until the heat breaks in the afternoon. The big market in the nearest town is every Wednesday. In the early afternoon of every Friday, the men of the village go to the mosque to worship together. Muslim holidays are announced by the moon’s phase and ratified by the authority of the marabouts, whose dictum mainly spreads by radio and word of mouth. When I called a meeting, planned an event, or set up a time to talk with someone, I did so by making reference to the prayer times, and I limited myself to days that can easily be described in the Wolof language: today, tomorrow, next week.
It is clear, then, that the system of calling to make an appointment would simply not work here. Instead, people walk or ride in to Ndiago in the early morning, even before the health post is open. They take their seats on the benches and wait, the seats around them filling up quickly. As each person walks in, perhaps with a child slung across her back or guiding an elderly relative, he or she pauses to acknowledge those who are already seated. Each newcomer greets, asks after the health of common friends or relatives in neighboring villages, and finds a place to sit. The greeting ritual is so highly formalized that someone who is seriously ill will, when asked about his or her health, respond that everything is in perfect shape. Nobody is a stranger here. The men and women talk about recent events in the villages: last week’s baptisms, the soccer matches between the young men, the peanut harvest. Back at home, in doctors’ offices across America, patients awkwardly sit with at least one empty seat between them and their unknown temporary neighbors. No conversation, no eye contact, no greetings. But in Ndiago, there is no physical space for avoidance in this waiting room.
All this is true, of course, in a lot of public places in Senegal, for example: schools and public transit. You are squished together with a lot of strangers, so you might as well make conversation. If the physical reality of the situation is such that it is impossible to feel the peace of solitude, you may as well give up denying that you are not alone. But there in that waiting room, where people come with sometimes terrifying illnesses, the crowd used to seem invasive to me. If you are scared for yourself, your child, or your parent, maybe the greeting ritual and patter of conversation grates at your nerves. If something you do not understand is making you sick, maybe what you want is a little bit of solitude and quiet to think it through. You are dealing with apprehension, fear, pain, and a whole host of other emotions. It could be difficult to sort those things out while diligently taking part in a description of all the gifts given on the occasion of a recent wedding.
But this is where Senegalese and American cultures clash, and this is where the waiting room—which at first struck me as a bizarrely and inappropriately transferred Western concept—starts to look like a perfectly designed space for the role it has to play. No one in Senegal seeks out solitude, unless they are very elderly and choose to spend most of their time in prayer and preparation for death. No one chooses to strike off into the wilderness alone, far from family and friends. I used to see solitude in Senegal as something to be avoided for practical reasons: the community of the village supports and sustains all the individuals within it, and no individual could survive for long without its framework. But maybe such a closeness is also an emotional necessity for the patients in the Ndiago waiting room. To be alone is to accept that your death is coming, or to seek it out prematurely. Whereas in a time of sickness, a crowded waiting room where you sit elbow-to-elbow with neighbors and acquaintances would be reassuring. All those people squished in next to you are your life, your way of continuing to live. The doctor and his medications might provide some help and comfort, but I think there is a way in which a return to health and well-being starts here, in this waiting room, where it is impossible to be alone, and so perhaps impossible to die.
JESSIE SEILER is a first year medical student. She served as a Peace Corps Volunteer in Senegal before beginning her medical education. A native of Los Angeles and graduate of St. John’s College in Annapolis, MD, she hopes for a career practicing and teaching medicine in developing countries.

Leave a Reply