Andrea Meyerhoff
Baltimore, Maryland, United States
 |
|
|
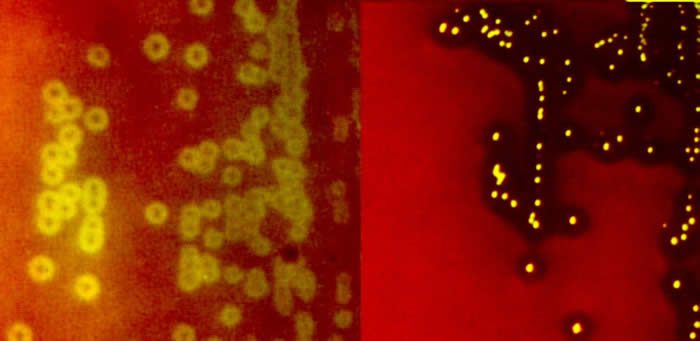
Alpha and Beta hemolytic streptococci grown on blood agar |
I respect the streptococcus. It is a bacterium—a whole genus of them—that excels at making people sick. It may shape a childhood understanding of illness, rupture ties that bind a family, or drive an appreciation for a great moment of human achievement. More recently, however, the memory of a particular streptococcus made me realize how far we have not come.
The genus Streptococcus was named for its microscopic appearance. When colored with Gram’s stain, it shows up as a string of round, purple beads. Classically educated 19th century bacteriologists named it as the Greeks would have, if they’d had microscopes. The organism’s shape is a sphere (Gr. coccus), with the spheres arranged in a twisted chain (Gr. strepto).
If I adjust the knobs of the microscope and these creatures come into view, I admit to a certain pleasure. To an infectious disease doctor their appearance is familiar, almost endearing, in a clumsy, Fred Flintstone kind of way. But it is easy to be fooled.
Despite their rock-like appearance, streptococci are remarkably good at reproduction, survival, and tissue destruction—important qualifications in this rough and tumble Age of Man. There are over 200 species that cause human disease; they can invade just about any tissue. In the pre-antibiotic 1930s, a healthy young adult with streptococcus in the blood had an 80 percent chance of dying. By the 1970s, a few decades of penicillin use had caused this figure to drop to 15 percent. Streptococcus has lost a lot of clout.
Some members of the genus are members of an alphabetic series, the Lancefield classification, which runs at least to the letter V. This is far more streptococci than I ever got to know since it’s mostly the beginning of the alphabet that involves itself in human disease.
The classic is group A strep. In the pre-antibiotic era it was the cause of many diseases, among them puerperal sepsis, or childbed fever. This disease was responsible for the deaths of millions of healthy, young women whose families recall them only as having “died in childbirth.” Particularly tragic is the 1847 discovery by Austrian obstetrician Ignaz Semmelweis that simple handwashing could prevent the spread of this fatal illness. When he published his findings, Semmelweis was ridiculed and dismissed from his hospital position. He was then committed to a psychiatric hospital where he died shortly after admission.
There are other landmark dates in the story of group A strep. In 1928 London, bacteriologist Alexander Fleming noticed how well a stray Penicillium mold prevented bacterial growth on a Petri dish. It took several years and a world war to find support for the work of Ernst Chain and Howard Florey, who sought to isolate a drug and produce quantities for use in sick patients. But by the 1944 D-day invasion of Europe, enough penicillin had been produced to substantially reduce deaths and amputations from battlefield injuries. The 1945 Nobel Prize in Medicine was awarded to Drs. Fleming, Chain, and Florey for the discovery of penicillin.
Not publicly documented in the history of group A streptococcus or penicillin is the 1934 birth of my mother at Boston City Hospital. At the time her own mother was a healthy twenty-six-year-old. Shortly after her daughter’s birth, my grandmother developed a fever. What my mother knows is that the fever was due to an infection common among healthy, young mothers at the time and that her mother died soon after.
About fifty years later, I trained at City. Founded in 1864 to care for the poor, Boston City, along with New York’s Bellevue and Chicago’s Cook County Hospitals, were said by the mid-20th century to have trained almost half the doctors in the US. Boston City’s buildings have since been demolished, but when I was there in the 1980s, a few of the floors were still the old-fashioned, open Nightingale wards. Once in a while when I hurried through, I imagined older furniture—white-painted, iron-rail beds lined up in rows against the long walls. In the middle of a row, sitting up in bed with her hair combed and her baby in her arms, might be my grandmother—for a brief moment appearing no different from the other smiling new mothers.
The daughter of immigrants, my grandmother was a modern woman. She believed that women should have the vote; she was the first member of her family to go to college. But she missed penicillin by about ten years. In the 1940s, Boston City’s Thorndike Memorial Laboratory was where a giant of infectious disease, Maxwell Finland, did much of the early work on penicillin. Professor Finland, whom I am proud to say I met, joined the Thorndike in 1929. He was known for the respect he showed even the poorest patients. So even if she missed penicillin, there was a chance my grandmother was seen by young Dr. Finland. I like to think so.
It is probably no surprise that after group A streptococcus comes group B, a cause of serious infections in those with compromised immune systems. Textbooks describe it as “indolent,” though I think this is all relative. A nasty strep B meningitis killed a young diabetic patient of mine, causing me to handle this organism with care despite its reputation as a slacker.
Few board exams neglect to ask which streptococcus, when grown from the patient’s blood, is associated with colon cancer. The answer is group D. The examinee is usually required to undertake a thorough search for malignancy before leaving the test question. Innumerable exam questions notwithstanding, I’ve never seen a patient whose blood cultures grew strep D who was also found to have colon cancer. This is a good thing; strep D is enough of a problem on its own.
Once in a while, a throat, swabbed to test for the fearsome group A, grows a group C or G strep instead. For the most part these rare organisms are innocent bystanders. But there is the occasional patient population in whom strep C or G may cause real trouble—for instance, women who have had a mastectomy. Surgery or radiation treatment can damage the lymphatic vessels. The scarring results in impaired drainage and a chronically red, swollen arm. Such tissue is attractive to streps C and G. Infection is tricky to detect because the anatomy is already abnormal, but the patient usually responds well after a few days of treatment with penicillin or a related drug. As a fellow I found streps like C and G among the best of microbiologic curiosities, interesting and easy to cure.
One day near the end of my fellowship, one of the oncologists asked me to see a patient in the emergency room. He was a man in his early fifties, diagnosed a couple of years earlier with lymphoma. He’d already visited the ER a couple of times for redness and swelling in his neck. Now he was back with a fever. His face was pale, his dark hair starting to gray. He was young for his tumor type. His chart said he had advanced disease, previous surgery, and radiation. Some time ago he’d owned a company with hundreds of employees.
Polite and informative in response to questions, his skin was hot, his temperature over 103º F. The left side of his neck was red, swollen, and hard to the touch—scar tissue with after-effects of radiation. As we talked I noticed that the whites of his eyes were visible above the iris. Maybe it was the rapid weight loss of advanced malignancy, or maybe it was anxiety. His heart was racing at about 120 beats per minute. He had a thorough grasp of his illness, treatments, recent trips to the emergency room—what you’d expect from an effective executive. He asked me if I knew where his doctor was. I said he was on his way.
As I finished the physical exam, someone handed me the results of blood cultures taken a few days earlier. I glanced at the sheet. The patient’s blood was growing something I’d never seen before—a group F streptococcus. The antibiotic tests said the bug was susceptible to everything, including penicillin. Though exotic, strep F was pretty tame. But it had made it into the normally sterile blood stream, one of the most protected compartments of the body—by definition, a life-threatening emergency. In the silence, the patient’s face shone with sweat; his eyes were huge.
We would start, I told the patient, by pushing the gas pedal to the floor. Strong antibiotics, right away. His face relaxed, so I thought he liked the idea. I did. After a call to the oncologist, I returned to the bedside to check medications, allergies, kidney function—the usual laundry list before starting a new drug. The patient’s wife came in to say she would return shortly. The patient asked again when his oncologist was coming; his heart was now slamming away at 140 beats per minute.
I was sitting in a corner of the alcove writing up the consultation when the alarm on the IV pump brought me to the bedside. That’s when he asked me to talk to him.
It’s hard to emerge from the revelation of group F strep, a life-threatening infection, a string of complicated dose calculations, and all the other million things we like to think prevent a relentless tide from lapping higher on the beach. I looked at him again and recognized someone who didn’t underestimate the tide. He was so scared that even a preoccupied fellow could be company. I pulled up a chair.
We talked at length about streptococci and penicillin, but he seemed to want to talk about something larger. This is very difficult to do with a patient you’ve just met. He was graceful and didn’t press the issue. I saw a flash of a skilled negotiator, someone who was used to biding his time. But on my end, the streptococcus weighed heavily. His chances were slim. Talking about it was part of the job. We warmed up to the subject slowly, with my stalling on the easy stuff—the original diagnosis, his decision to leave work. He made a quick reference to his wife that made him turn his head away.
When his oncologist arrived, I left. About 30 minutes later, he died. When the oncologist told me, all I could do was hope that their conversation had progressed beyond the eccentricities of streptococcus F.
Epilogue
Once a feared killer that hovered at the edges of everlasting sadness, streptococcus became an organism easily dispatched with a brisk order for penicillin. But the world is not a static place, and as we’ve asserted a cranial capacity superior to that of the streptococcus, so we’ve also opened new doors through which this bug can invade and destroy human tissue. The better we get at keeping patients alive, the more we provide organisms like strep a weakened host in whom to cause disease. And in the race between human ingenuity and bacterial evolution, we are never the sure winner.
So streptococcus may still tear around the normally fortified bloodstream, driving a breathless tachycardia for which we can do little more than count. This humdrum, round bug can demand we abandon our numbers and gadgets and instead use some very old tools which, as strep F showed, will rust if left too long unused.
ANDREA MEYERHOFF, MD is an infectious disease physician and former Fulbright scholar. Previously a counterterrorism official in the US government, she is now a member of the faculty of Johns Hopkins School of Medicine and head of GexGroup, Inc, a drug development and communications firm. Her writing has appeared in the New York Times, Washington Post, several newspapers via McClatchy News, as well as peer reviewed medical literature.
Highlighted in Frontispiece Spring 2011 – Volume 3, Issue 2
Spring 2011 | Sections | Infectious Diseases

Leave a Reply